Antibiotics transformed modern medicine by making it possible to treat bacterial infections that were once deadly. However, over time many bacteria have developed the ability to survive these drugs. This phenomenon is known as antibiotic resistance.
Antibiotic resistance occurs when bacterial populations evolve mechanisms that allow them to withstand medications designed to kill them or stop their growth. As resistant bacteria spread, infections become harder to treat and require stronger or alternative medications.
Understanding how antibiotic resistance develops and spreads within bacterial populations is essential for protecting global health and preserving the effectiveness of antibiotics.
What Is Antibiotic Resistance?
Antibiotic resistance is the ability of bacteria to survive exposure to antibiotics that would normally kill them or inhibit their growth.
Resistance occurs because bacteria can acquire genetic traits that protect them from the drug’s effects.
These traits may allow bacteria to:
- Destroy the antibiotic
- Prevent the drug from entering the cell
- Pump the drug out of the cell
- Modify the antibiotic’s target inside the bacterium
When resistant bacteria survive treatment, they continue reproducing and pass resistance traits to future generations.
How Antibiotic Resistance Develops
Antibiotic resistance develops through evolution and genetic change within bacterial populations.
Two major processes contribute to this development:
Genetic Mutations
Random mutations in bacterial DNA may produce changes that allow bacteria to survive antibiotic exposure.
If the mutation provides protection, those bacteria survive and reproduce while susceptible bacteria die.
Over time, resistant bacteria become more common within the population.
Horizontal Gene Transfer
Bacteria can also acquire resistance genes from other bacteria through horizontal gene transfer.
This process allows genes to move between cells using mechanisms such as:
- Conjugation
- Transformation
- Transduction
Because of horizontal gene transfer, resistance can spread rapidly across different bacterial species.
The Role of Natural Selection
Antibiotic resistance is a classic example of natural selection.
When antibiotics are used:
- Most susceptible bacteria are killed.
- Resistant bacteria survive.
- The surviving bacteria reproduce.
- The resistant population grows.
Over time, the bacterial community becomes dominated by resistant strains.
This process can occur quickly because bacteria reproduce rapidly.
Common Mechanisms of Antibiotic Resistance
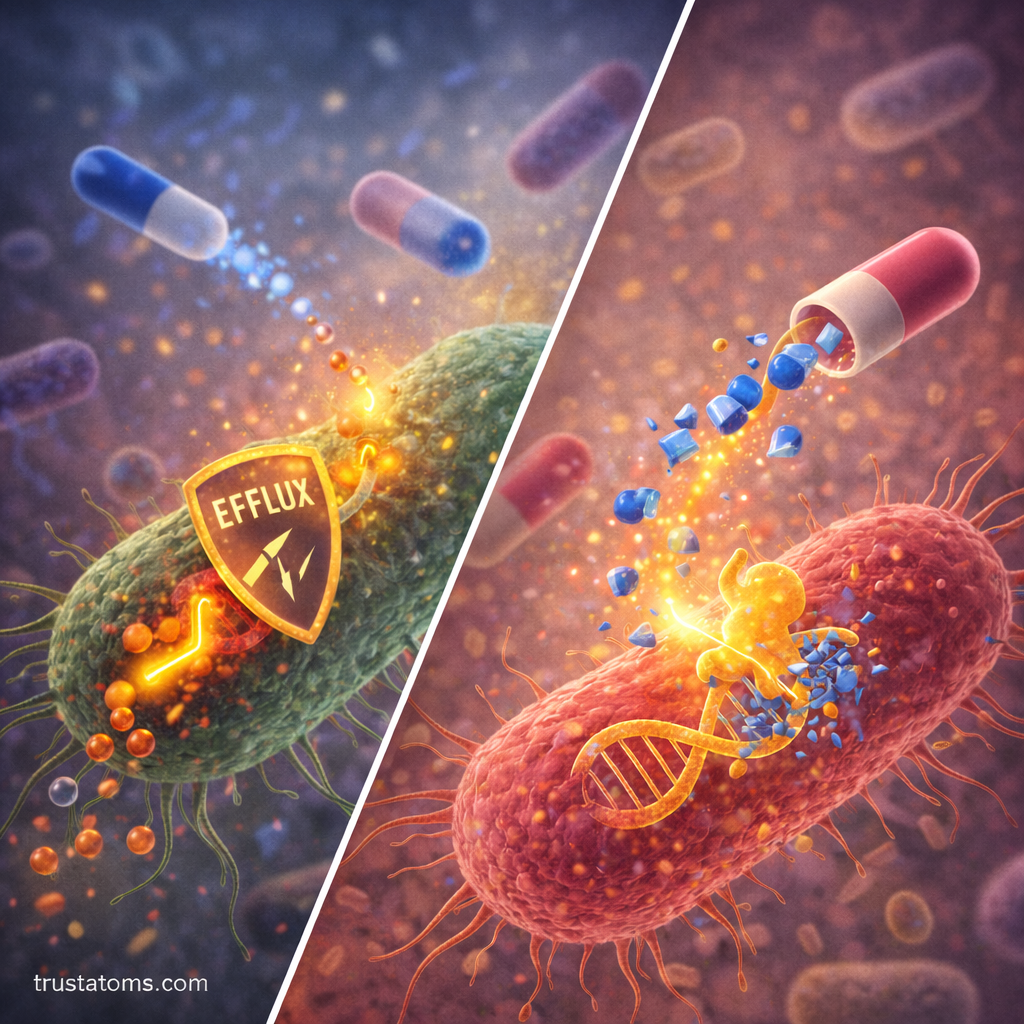
Bacteria use several biological strategies to survive antibiotic exposure.
Enzyme Production
Some bacteria produce enzymes that break down antibiotics.
For example:
- Beta-lactamase enzymes destroy penicillin-type antibiotics.
These enzymes neutralize the drug before it can affect the bacterial cell.
Target Modification
Antibiotics often work by binding to specific molecules inside bacterial cells.
Some bacteria alter these target molecules so the antibiotic can no longer attach effectively.
This prevents the drug from interfering with bacterial processes.
Efflux Pumps
Certain bacteria possess efflux pumps, which are proteins that actively push antibiotics out of the cell.
By removing the drug, the bacteria prevent it from reaching harmful concentrations.
Reduced Cell Permeability
Some bacteria change the structure of their cell membrane or cell wall to prevent antibiotics from entering the cell.
This acts as a protective barrier against the drug.
Horizontal Gene Transfer and Resistance Spread
Horizontal gene transfer plays a major role in spreading antibiotic resistance within bacterial populations.
Resistance genes can move between bacteria through mobile genetic elements such as:
- Plasmids
- Transposons
- Integrons
These DNA elements carry resistance genes and allow them to spread quickly between cells.
This exchange can occur even between different bacterial species.
Because of this, a resistance gene that appears in one bacterium may eventually spread across many types of bacteria.
Antibiotic Resistance in Healthcare Settings
Hospitals and healthcare facilities are environments where antibiotic resistance often emerges.
Several factors contribute to this:
- Frequent antibiotic use
- High patient density
- Vulnerable immune systems
- Opportunities for bacterial transmission
These conditions create strong selective pressure for resistant bacteria.
Examples of well-known resistant bacteria include:
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Drug-resistant Mycobacterium tuberculosis
- Carbapenem-resistant Enterobacteriaceae
These infections can be difficult to treat and require specialized medical care.
Antibiotic Resistance in Agriculture
Antibiotics are sometimes used in livestock production to prevent disease and promote growth.
However, this practice can contribute to the development of resistant bacteria.
These bacteria may spread through:
- Food products
- Water contamination
- Environmental exposure
- Direct contact with animals
Reducing unnecessary antibiotic use in agriculture is an important step in slowing resistance development.
Global Consequences of Antibiotic Resistance
Antibiotic resistance poses a growing challenge for healthcare systems worldwide.
Major consequences include:
Harder-to-Treat Infections
Resistant infections may require:
- Stronger medications
- Longer treatment periods
- Combination therapies
Increased Healthcare Costs
Treating resistant infections often involves longer hospital stays and more expensive medications.
Higher Mortality Rates
When infections cannot be treated effectively, they can become life-threatening.
Reduced Effectiveness of Medical Procedures
Many medical procedures depend on effective antibiotics to prevent infection, including:
- Surgery
- Organ transplantation
- Cancer treatments
Without effective antibiotics, these procedures become much riskier.
Strategies to Combat Antibiotic Resistance
Scientists, healthcare professionals, and policymakers are working to slow the spread of resistance.
Key strategies include:
Responsible Antibiotic Use
Doctors aim to prescribe antibiotics only when necessary and ensure patients complete full treatment courses.
Infection Prevention
Preventing infections reduces the need for antibiotics.
Important measures include:
- Vaccination
- Proper hygiene
- Sterilization in healthcare settings
Antibiotic Stewardship Programs
Hospitals implement programs that guide the appropriate use of antibiotics.
These programs help reduce unnecessary prescriptions.
Development of New Antibiotics
Researchers are developing new antimicrobial drugs and alternative treatments to combat resistant bacteria.
The Role of Research and Surveillance
Monitoring antibiotic resistance is essential for controlling its spread.
Scientists track resistance patterns by:
- Sequencing bacterial genomes
- Monitoring infection outbreaks
- Analyzing resistance genes in microbial populations
This information helps guide treatment strategies and public health policies.
Final Thoughts
Antibiotic resistance in bacterial populations illustrates how quickly microorganisms can evolve in response to environmental pressures. Through genetic mutations and gene transfer, bacteria develop new ways to survive medications designed to eliminate them.
While antibiotic resistance presents significant challenges, understanding the biological mechanisms behind it provides opportunities to develop new treatments and prevention strategies.
Responsible antibiotic use, continued scientific research, and global cooperation will play essential roles in protecting the effectiveness of antibiotics for future generations.