The adaptive immune system is responsible for targeted, long-lasting protection against specific pathogens. Unlike the innate immune system, which responds quickly but broadly, the adaptive response is highly precise and capable of remembering past infections.
At the center of this process are activation pathways—a series of coordinated steps that allow immune cells to recognize threats, communicate, and mount an effective defense.
Understanding adaptive response activation pathways helps explain how the body develops immunity, responds to vaccines, and fights infections with precision.
What Is the Adaptive Immune Response?
The adaptive immune response is a specialized defense system that:
- Targets specific pathogens
- Improves with repeated exposure
- Creates immunological memory
It primarily involves:
- T lymphocytes (T cells)
- B lymphocytes (B cells)
These cells are activated through carefully regulated pathways that ensure accurate and efficient immune responses.
Key Steps in Adaptive Immune Activation
Adaptive immunity follows a structured sequence of events.
1. Antigen Recognition
The process begins when immune cells detect a foreign antigen.
- Antigens are fragments of pathogens (e.g., proteins from viruses or bacteria)
- Recognized by specific receptors on T cells and B cells
- Each lymphocyte is programmed to recognize a unique antigen
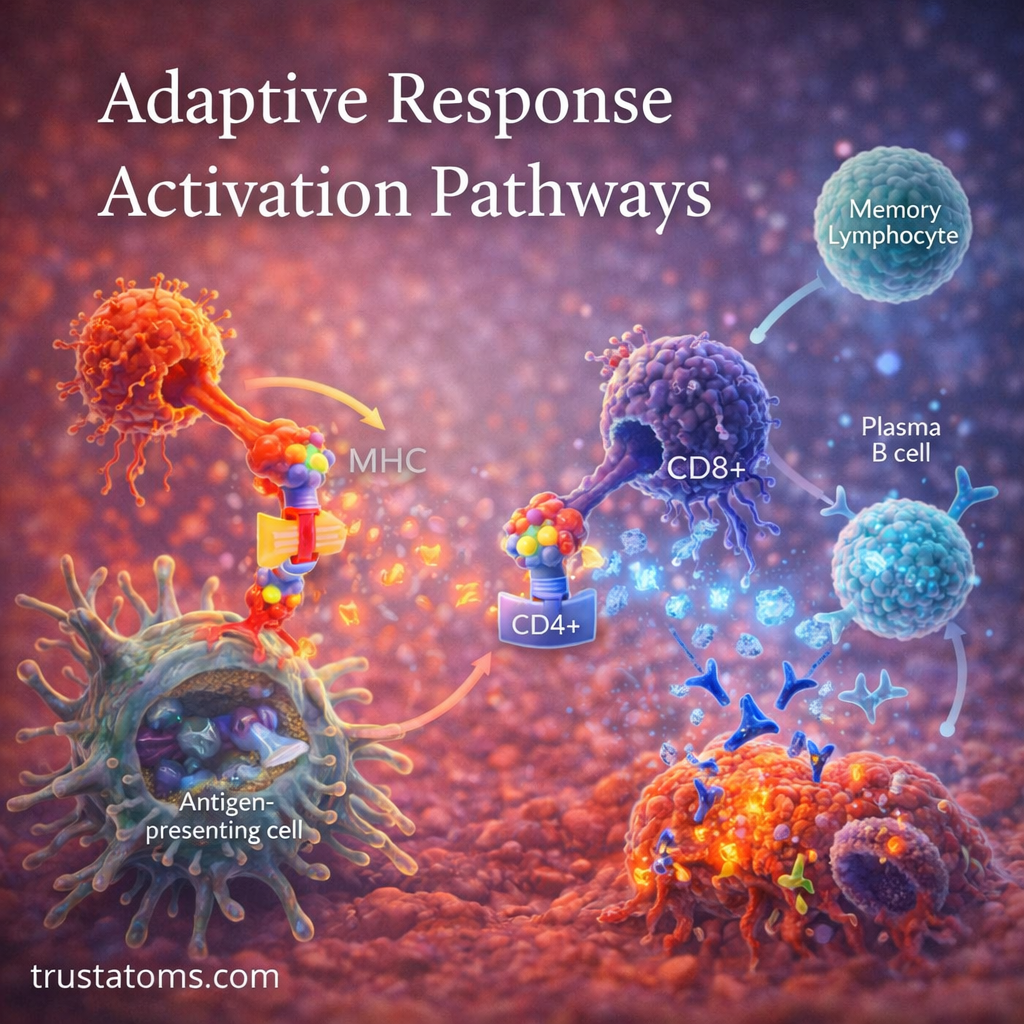
2. Antigen Presentation
Antigen-presenting cells (APCs), such as dendritic cells, play a critical role.
- Capture and process pathogens
- Present antigen fragments on their surface
- Use MHC molecules to display these fragments
This step bridges innate and adaptive immunity.
3. T Cell Activation
T cells require multiple signals to become fully activated.
Signal 1: Antigen Recognition
- T cell receptors (TCRs) bind to antigen-MHC complexes
Signal 2: Co-stimulation
- Additional signals from APCs confirm the presence of a real threat
- Prevents accidental activation
Signal 3: Cytokine Signaling
- Cytokines guide T cell differentiation and response type
4. Clonal Expansion
Once activated, T cells and B cells rapidly multiply.
- Produces many identical cells (clones)
- Ensures a strong and efficient immune response
- Expands cells specific to the detected antigen
5. Differentiation
Activated immune cells develop into specialized types.
T Cells:
- Helper T cells (CD4+): Coordinate immune responses
- Cytotoxic T cells (CD8+): Destroy infected cells
- Regulatory T cells: Control immune activity
B Cells:
- Differentiate into plasma cells
- Produce antibodies targeting specific antigens
6. Effector Response
Effector cells carry out the immune attack.
- Cytotoxic T cells kill infected cells
- Antibodies neutralize pathogens
- Helper T cells activate other immune cells
7. Memory Formation
After the infection is cleared:
- Some cells become memory cells
- Remain in the body long-term
- Enable faster and stronger responses upon re-exposure
T Cell Activation Pathway
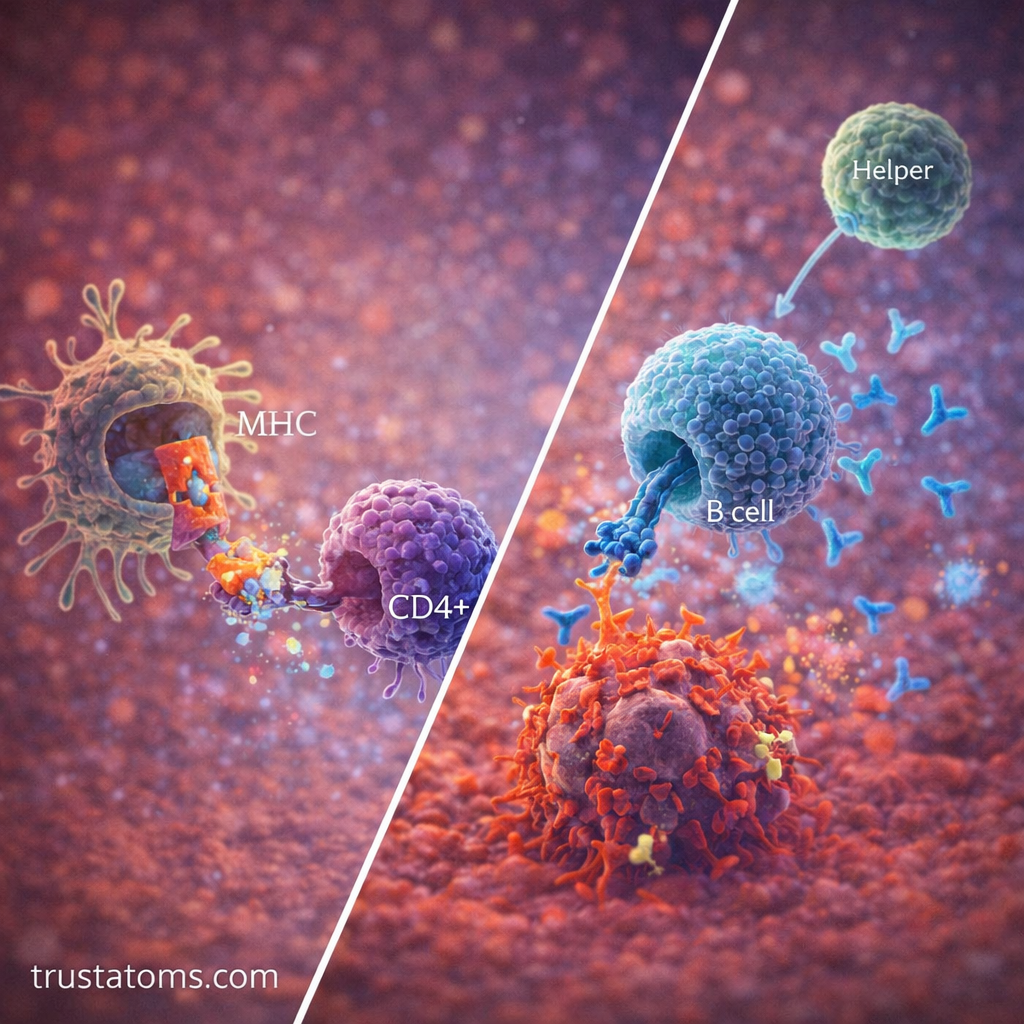
T cells are central to adaptive immunity and follow a precise activation pathway.
Key Components:
- T cell receptor (TCR)
- MHC molecules on APCs
- Co-stimulatory signals
- Cytokines
Activation Flow:
- APC presents antigen via MHC
- TCR recognizes antigen-MHC complex
- Co-stimulatory signals confirm activation
- Cytokines direct differentiation
- Activated T cells proliferate and specialize
B Cell Activation Pathway
B cells are responsible for antibody production and can be activated in two ways.
T-Dependent Activation
Requires help from helper T cells.
Steps:
- B cell binds antigen directly
- Presents antigen to helper T cell
- Receives activation signals from T cell
- Undergoes clonal expansion and differentiation
This pathway produces:
- Stronger immune responses
- Long-lasting memory
T-Independent Activation
Occurs without T cell assistance.
- Triggered by certain antigens (e.g., repeating structures on bacteria)
- Produces a faster but less durable response
- Limited memory formation
Role of Cytokines in Activation Pathways
Cytokines are essential signaling molecules that regulate immune responses.
They:
- Guide T cell differentiation
- Enhance or suppress immune activity
- Coordinate communication between cells
Examples of cytokine roles:
- Promoting inflammation
- Supporting antibody production
- Controlling immune intensity
Importance of Co-Stimulation
Co-stimulation ensures that immune responses are appropriate.
Why It Matters:
- Prevents accidental activation against self-antigens
- Confirms the presence of a real threat
- Adds an extra layer of immune control
Without co-stimulation, T cells may become inactive (anergic).
Adaptive Immunity vs Innate Immunity
Adaptive Immunity:
- Specific and targeted
- Slower initial response
- Develops memory
Innate Immunity:
- Rapid and non-specific
- First line of defense
- No long-term memory
Both systems work together to protect the body.
When Activation Pathways Go Wrong
Errors in adaptive immune activation can lead to disease.
Autoimmune Disorders
- Immune system attacks healthy tissues
- Caused by failure in self-recognition or regulation
Immunodeficiency
- Weak or absent immune response
- Increased susceptibility to infections
Chronic Inflammation
- Overactive immune pathways
- Persistent tissue damage
Key Functions of Adaptive Activation Pathways
- Recognize specific antigens
- Activate and expand immune cells
- Coordinate immune responses
- Produce antibodies
- Generate immune memory
- Maintain immune precision
Why Adaptive Activation Pathways Matter
These pathways ensure that the immune system responds accurately and efficiently.
They allow the body to:
- Fight infections with precision
- Avoid unnecessary damage to healthy tissues
- Build long-term protection against recurring threats
This is the foundation of vaccination and long-term immunity.
Final Thoughts
Adaptive response activation pathways are the backbone of targeted immunity. Through a series of carefully controlled steps, the immune system identifies threats, activates the right cells, and eliminates pathogens with precision.
Equally important, these pathways create memory that protects the body in the future. When functioning correctly, they provide powerful and long-lasting defense. When disrupted, they highlight how delicate and essential immune regulation truly is.
Understanding these pathways offers valuable insight into how the body defends itself—and how modern medicine can enhance or correct immune responses.