Calcium is one of the most important minerals in the human body, essential for muscle contraction, nerve signaling, blood clotting, and bone strength. Despite its many roles, calcium levels in the blood must remain within a very narrow range.
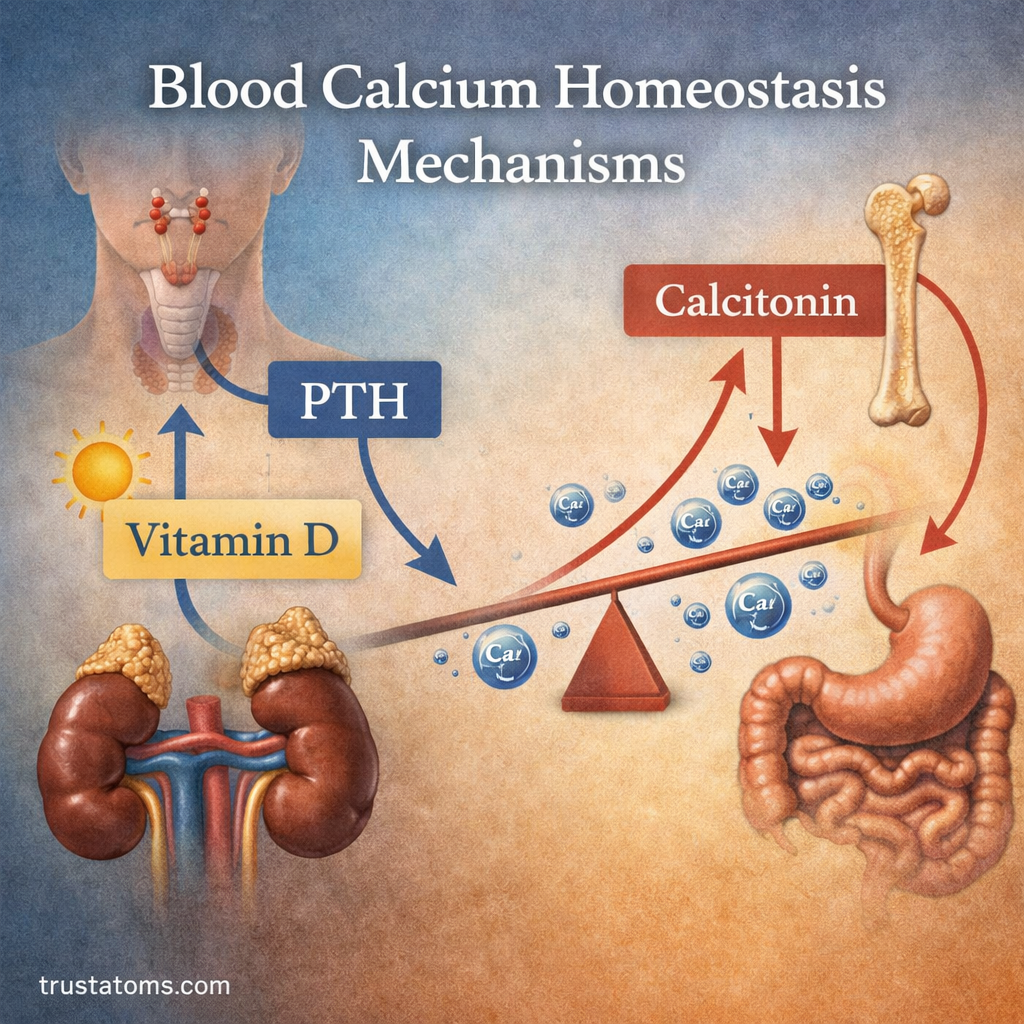
Blood calcium homeostasis refers to the processes that maintain stable calcium levels through coordinated actions of hormones, bones, kidneys, and the digestive system.
Why Calcium Balance Matters
Even small changes in blood calcium levels can disrupt critical bodily functions.
Key Roles of Calcium
- Muscle contraction (including the heart)
- Nerve impulse transmission
- Blood clotting
- Hormone secretion
- Structural support in bones and teeth
Because of these vital roles, the body tightly regulates calcium levels at all times.
Normal Blood Calcium Levels
The body maintains calcium within a narrow range:
- Approximately 8.5 to 10.5 mg/dL in adults
If levels fall outside this range, the body activates corrective mechanisms immediately.
Key Hormones in Calcium Regulation
Three primary hormones control blood calcium levels:
- Parathyroid hormone (PTH)
- Calcitonin
- Vitamin D (calcitriol)
These hormones work together to either increase or decrease calcium levels as needed.
Parathyroid Hormone (PTH): Raising Calcium Levels
PTH is the most important hormone for increasing blood calcium.
Where It Comes From
- Produced by the parathyroid glands
When It Is Released
- Triggered by low blood calcium levels
How PTH Works
PTH increases calcium through three main actions:
- Bone Resorption
- Stimulates release of calcium from bones
- Kidney Reabsorption
- Reduces calcium loss in urine
- Vitamin D Activation
- Enhances calcium absorption in the intestines
Vitamin D (Calcitriol): Enhancing Absorption
Vitamin D plays a supporting but critical role in calcium balance.
Activation Process
- Converted into active form (calcitriol) in the kidneys
- Stimulated by PTH
Main Function
- Increases calcium absorption from the digestive tract
Without sufficient vitamin D, the body cannot efficiently absorb dietary calcium.
Calcitonin: Lowering Calcium Levels
Calcitonin helps reduce blood calcium, although its role is less dominant than PTH.
Where It Comes From
- Produced by the thyroid gland
When It Is Released
- Triggered by high blood calcium levels
How Calcitonin Works
- Inhibits bone breakdown
- Promotes calcium storage in bones
- Slightly increases calcium excretion by the kidneys
Organs Involved in Calcium Homeostasis
Hormones act on specific organs to regulate calcium levels.
Bones: Calcium Storage
- Store about 99% of the body’s calcium
- Release calcium when levels are low
- Rebuild and store calcium when levels are high
Kidneys: Regulation and Excretion
- Filter calcium from the blood
- Reabsorb calcium when needed
- Activate vitamin D
Intestines: Absorption
- Absorb calcium from food
- Efficiency depends on vitamin D levels
Negative Feedback Mechanisms
Calcium regulation relies on feedback loops to maintain stability.
When Calcium Is Low
- Parathyroid glands release PTH
- Calcium is released from bones
- Kidneys conserve calcium
- Vitamin D increases absorption
- Blood calcium rises
When Calcium Is High
- Calcitonin is released
- Bone resorption decreases
- Calcium is stored in bones
- Blood calcium levels decrease
Calcium Homeostasis in Action
The system constantly adjusts based on the body’s needs.
Example Scenario
- Low dietary calcium intake → PTH increases → bones release calcium
- High calcium intake → calcitonin increases → calcium stored in bones
This dynamic balance ensures proper function without large fluctuations.
Disorders of Calcium Regulation
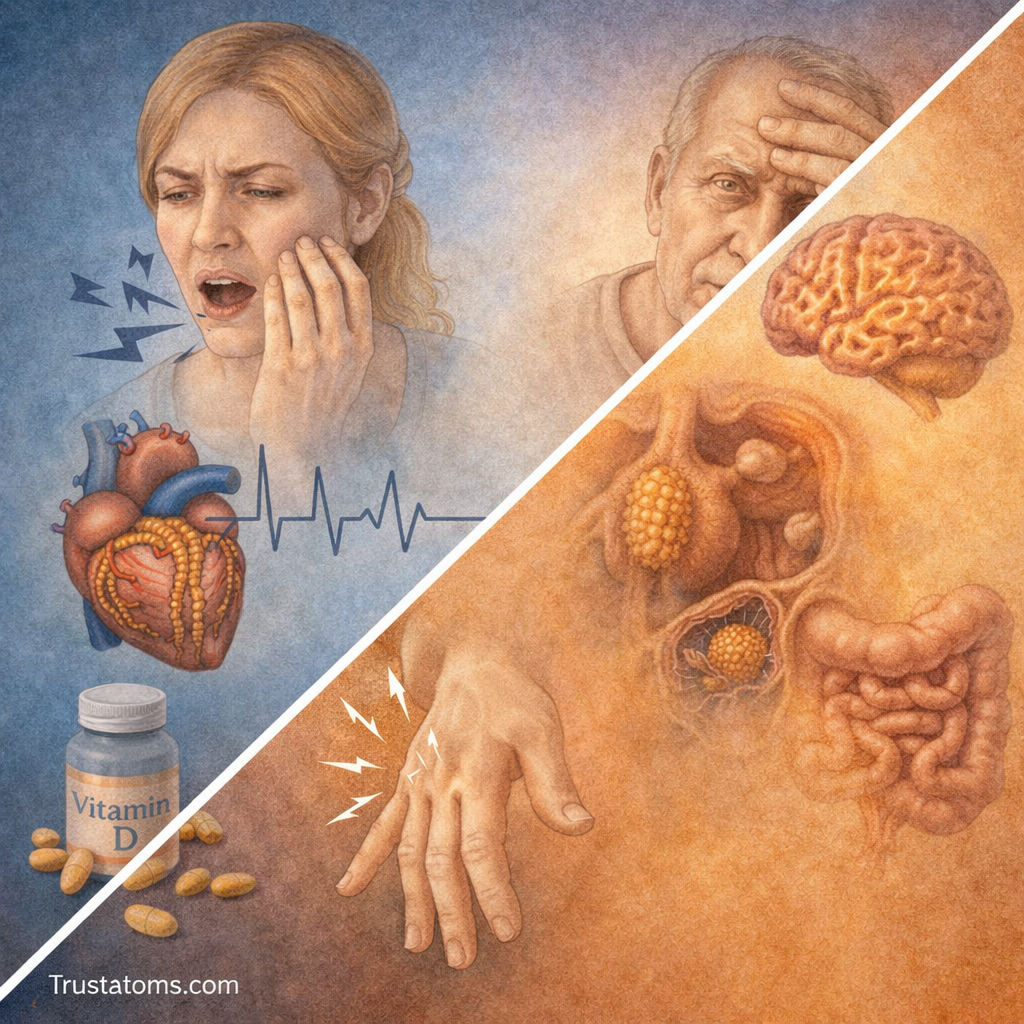
Imbalances in calcium homeostasis can lead to serious health issues.
Hypocalcemia (Low Calcium)
Symptoms:
- Muscle cramps
- Tingling sensations
- Irregular heartbeat
Causes:
- Low vitamin D
- Parathyroid dysfunction
- Kidney disease
Hypercalcemia (High Calcium)
Symptoms:
- Fatigue
- Kidney stones
- Confusion
Causes:
- Overactive parathyroid glands
- Excess vitamin D
- Certain cancers
Factors That Influence Calcium Balance
Several lifestyle and physiological factors affect calcium regulation.
Common Influences
- Diet: Adequate calcium intake is essential
- Vitamin D levels: Critical for absorption
- Hormones: Estrogen and others influence bone metabolism
- Age: Bone density changes over time
- Physical activity: Supports bone strength
Key Takeaways
- Blood calcium levels are tightly regulated
- PTH increases calcium, while calcitonin lowers it
- Vitamin D enhances calcium absorption
- Bones, kidneys, and intestines are key organs
- Feedback mechanisms maintain balance
- Imbalances can lead to serious health conditions
Final Thoughts
Blood calcium homeostasis is a finely tuned system that ensures stability in one of the body’s most essential minerals. Through hormonal signaling and organ coordination, the body maintains calcium levels within a narrow range necessary for survival.
Understanding these mechanisms highlights the importance of nutrition, hormonal balance, and overall health in maintaining proper calcium regulation.