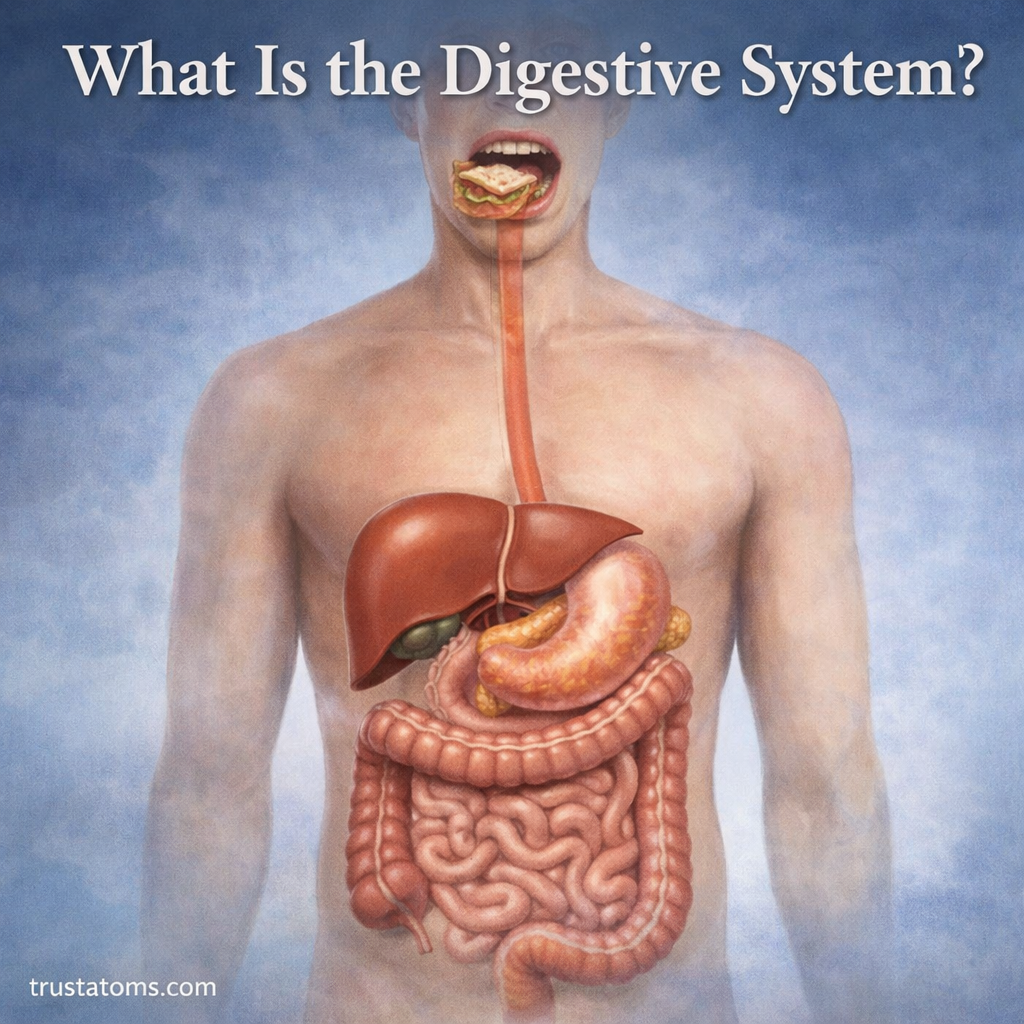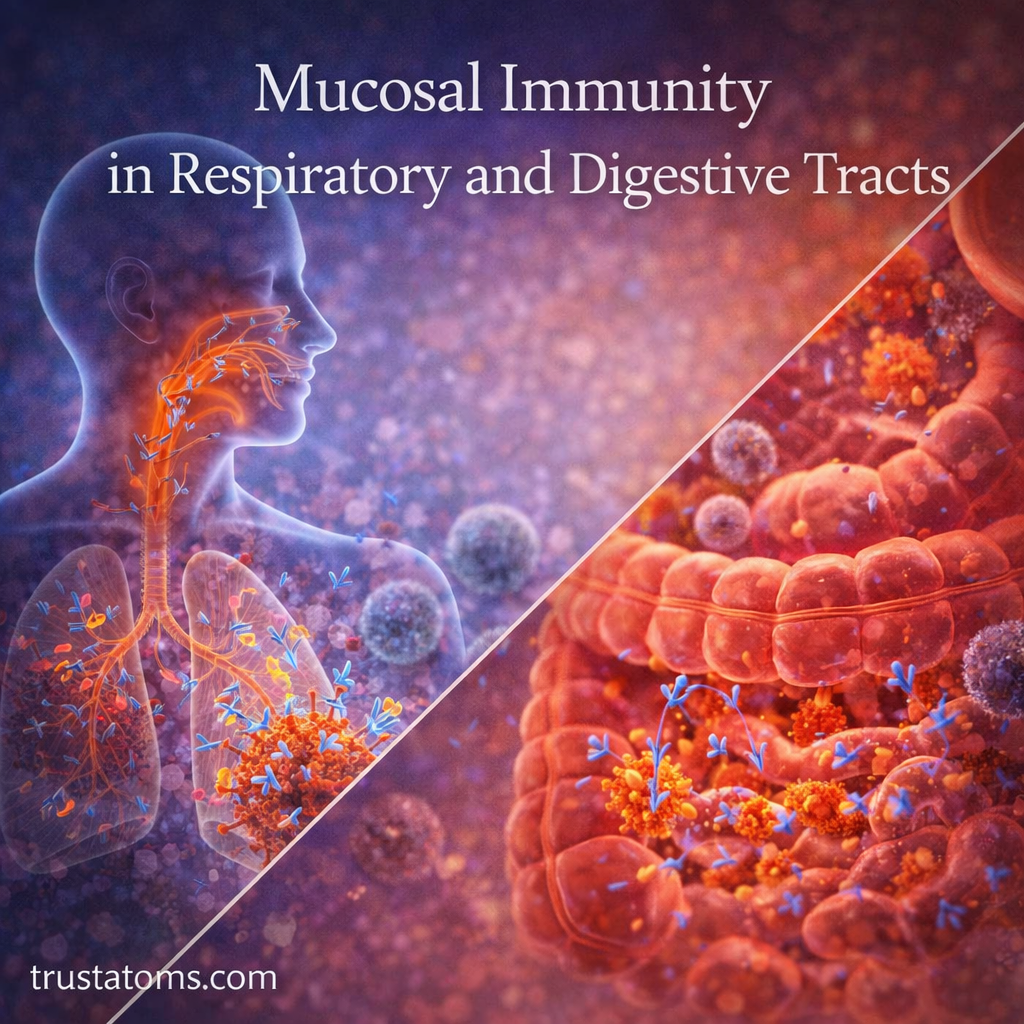
The body is constantly exposed to the outside environment through surfaces like the lungs and the digestive system. These areas, known as mucosal surfaces, are primary entry points for pathogens such as viruses, bacteria, and toxins.
To protect these vulnerable regions, the body relies on mucosal immunity—a specialized branch of the immune system designed to defend the respiratory and digestive tracts while maintaining balance with harmless substances.
What Is Mucosal Immunity?
Mucosal immunity refers to immune defenses located in mucous membranes that line:
- The respiratory tract (nose, throat, lungs)
- The digestive tract (stomach, intestines)
- Other areas such as the urogenital tract
These defenses must strike a balance:
- Protect against harmful pathogens
- Tolerate harmless substances like food and beneficial microbes
Key Components of Mucosal Immunity
Mucosal immunity involves both physical barriers and immune system elements working together.
Physical Barriers
These are the first line of defense.
- Mucus: Traps pathogens and particles
- Epithelial cells: Form a protective lining
- Cilia (in respiratory tract): Move mucus and trapped particles out
Immune Cells
Various immune cells are present within mucosal tissues.
- Macrophages
- Dendritic cells
- T cells
- B cells
These cells detect and respond to potential threats.
Antibodies (IgA)
The dominant antibody in mucosal immunity is Immunoglobulin A (IgA).
Functions of IgA:
- Binds to pathogens
- Prevents them from attaching to mucosal surfaces
- Neutralizes toxins
IgA is secreted directly into mucus, saliva, and intestinal fluids.
Mucosal Immunity in the Respiratory Tract
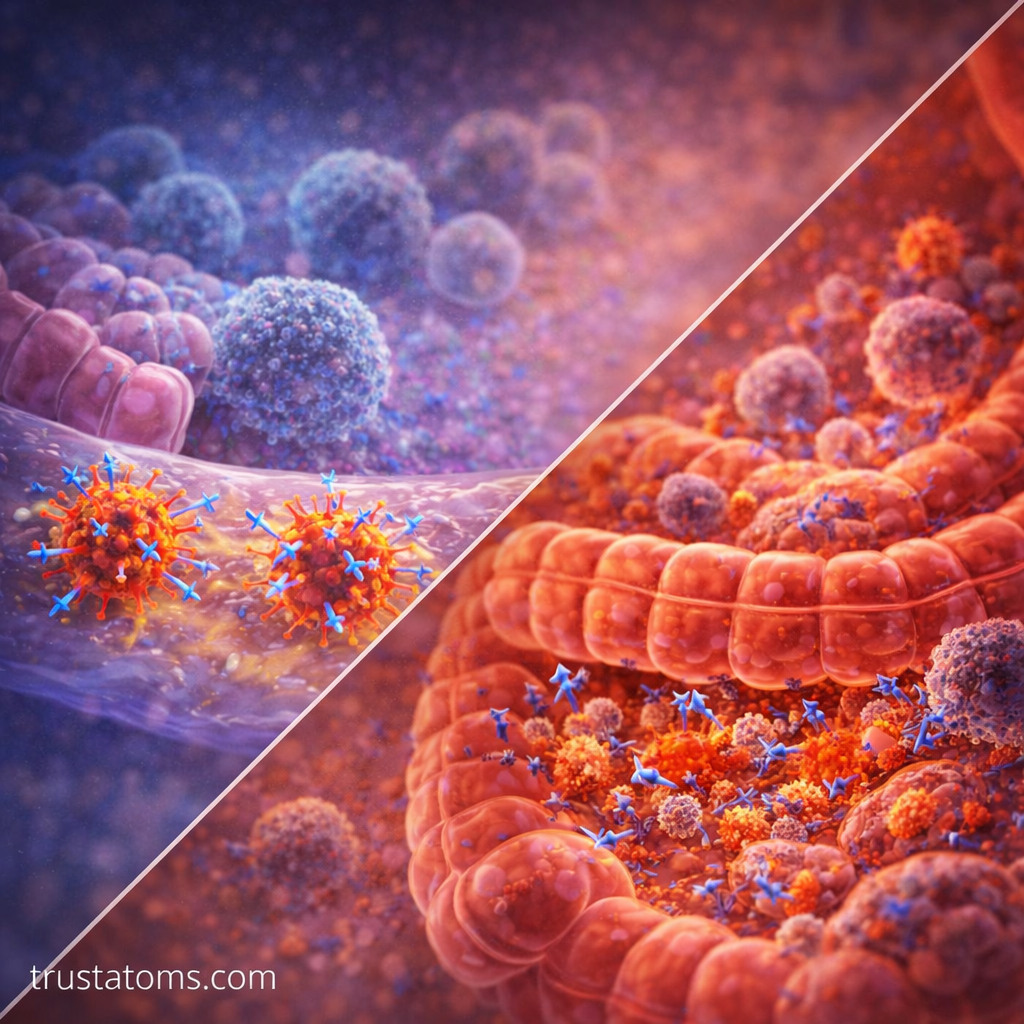
The respiratory system is constantly exposed to airborne particles and pathogens.
Defense Mechanisms:
- Mucus production traps inhaled particles
- Ciliary movement clears debris from airways
- Immune cells detect and eliminate pathogens
Immune Response in the Lungs
When pathogens enter:
- Dendritic cells capture and present antigens
- T cells are activated
- B cells produce IgA antibodies
- Pathogens are neutralized or removed
Importance
Mucosal immunity in the respiratory tract helps protect against:
- Viral infections (e.g., influenza)
- Bacterial infections
- Airborne allergens
Mucosal Immunity in the Digestive Tract
The digestive system faces a unique challenge: it must defend against pathogens while tolerating food and beneficial microbes.
Defense Mechanisms:
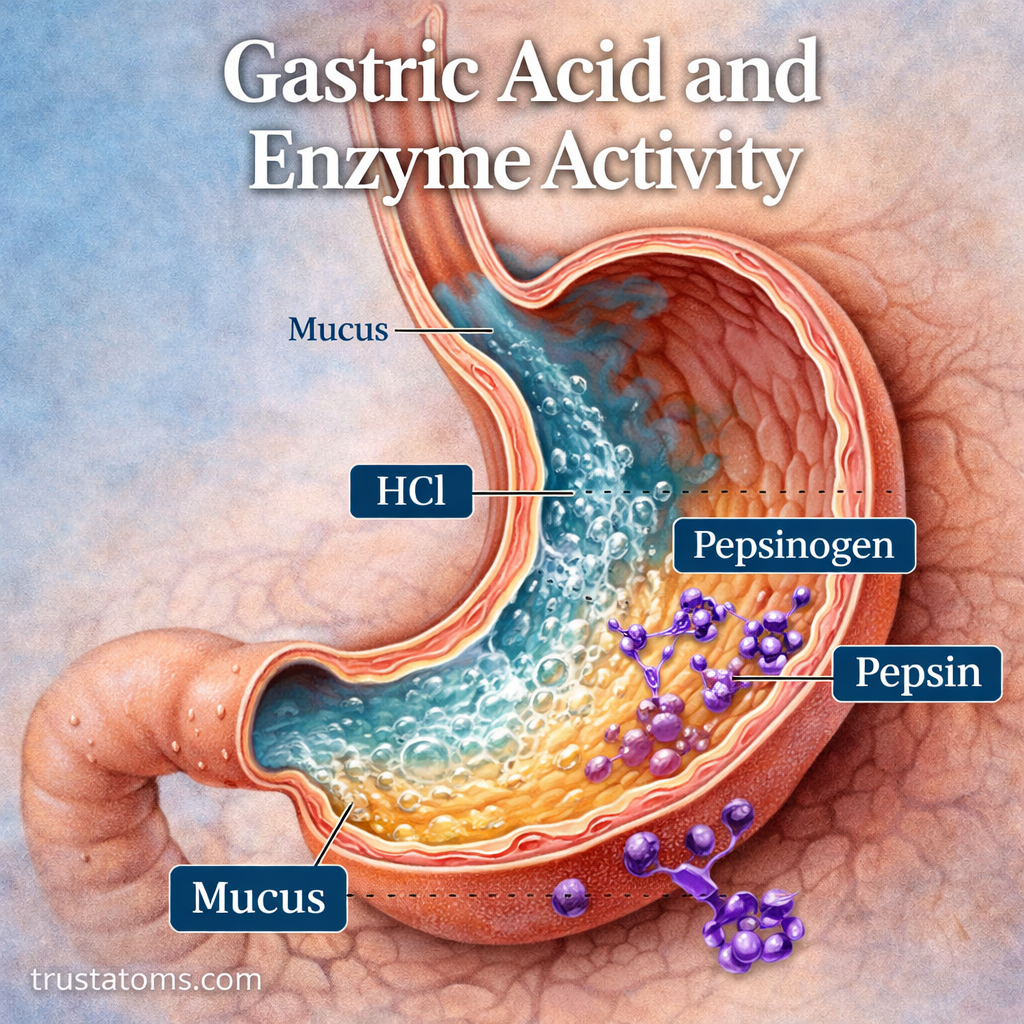
- Stomach acid destroys many pathogens
- Mucus lining protects intestinal walls
- Gut-associated lymphoid tissue (GALT) monitors immune activity
Role of Gut Microbiota
The gut contains trillions of beneficial microorganisms.
They:
- Compete with harmful pathogens
- Support immune system development
- Help regulate immune responses
Immune Response in the Intestines
- Antigens are sampled by specialized cells
- Dendritic cells present antigens to immune cells
- B cells produce IgA
- Immune responses are activated or suppressed as needed
Mucosal-Associated Lymphoid Tissue (MALT)
MALT is a key part of mucosal immunity.
It includes:
- Tonsils (respiratory tract)
- Peyer’s patches (small intestine)
- Appendix
Functions of MALT:
- Detect pathogens at mucosal surfaces
- Initiate immune responses
- Support antibody production
MALT acts as a surveillance system across mucosal tissues.
Balancing Defense and Tolerance
One of the most important features of mucosal immunity is its ability to balance protection and tolerance.
Why This Balance Matters:
- Prevents unnecessary immune reactions to food
- Maintains harmony with beneficial microbes
- Reduces risk of chronic inflammation
When Balance Is Disrupted:
- Allergies may develop
- Inflammatory diseases can occur (e.g., inflammatory bowel disease)
- Increased susceptibility to infections
Differences Between Respiratory and Digestive Mucosal Immunity
Respiratory Tract:
- Focuses on airborne threats
- Relies heavily on mucus and cilia
- Rapid clearance of pathogens
Digestive Tract:
- Handles ingested substances
- Requires tolerance to food and microbiota
- Involves complex immune regulation
Role in Vaccination
Mucosal immunity is an important target in vaccine development.
Mucosal Vaccines:
- Delivered through nasal sprays or oral routes
- Aim to generate IgA responses
- Provide localized protection at entry points
Benefits:
- Faster response at infection sites
- Reduced pathogen transmission
- Enhanced overall immunity
When Mucosal Immunity Fails
Problems in mucosal immunity can lead to various conditions.
Respiratory Issues:
- Chronic infections
- Asthma
- Allergic reactions
Digestive Disorders:
- Inflammatory bowel disease
- Food sensitivities
- Gut infections
Key Functions of Mucosal Immunity
- Protects major entry points of the body
- Traps and removes pathogens
- Produces IgA antibodies
- Maintains balance with microbiota
- Regulates immune responses
Why Mucosal Immunity Matters
Mucosal surfaces are constantly exposed to the external environment. Without specialized defenses, the body would be highly vulnerable to infection.
Mucosal immunity ensures that:
- Pathogens are stopped early
- Immune responses are controlled
- The body maintains internal balance
It is a critical component of overall immune health.
Final Thoughts
Mucosal immunity plays a vital role in protecting the respiratory and digestive systems—two of the body’s most exposed and vulnerable areas.
Through a combination of physical barriers, immune cells, and specialized antibodies, the body can defend against harmful invaders while maintaining tolerance to harmless substances.
This delicate balance is essential for both protection and long-term health, highlighting the importance of mucosal immunity in everyday life.