The immune system doesn’t rely on just one line of defense—it uses layered strategies that work together. One of the most powerful and often overlooked components is the complement system.
The complement system is a group of proteins in your blood that enhances (or “complements”) the ability of immune cells to fight infections. It plays a key role in both innate immunity and adaptive immunity, helping your body detect, attack, and clear harmful invaders.
What Is the Complement System?
The complement system consists of over 30 proteins found in blood plasma and on cell surfaces. These proteins circulate in an inactive state and become activated when the body detects a threat.
Main Purpose
- Enhance immune response
- Mark pathogens for destruction
- Directly kill certain microbes
- Promote inflammation
Think of the complement system as a biological amplifier—once triggered, it rapidly strengthens the immune response.
Why the Complement System Matters
Without the complement system, your immune defenses would be slower and less effective.
Key Benefits
- Speeds up pathogen recognition
- Improves efficiency of phagocytosis
- Helps eliminate bacteria and viruses
- Supports inflammation and immune signaling
It acts as a bridge between immediate defenses and targeted immune responses.
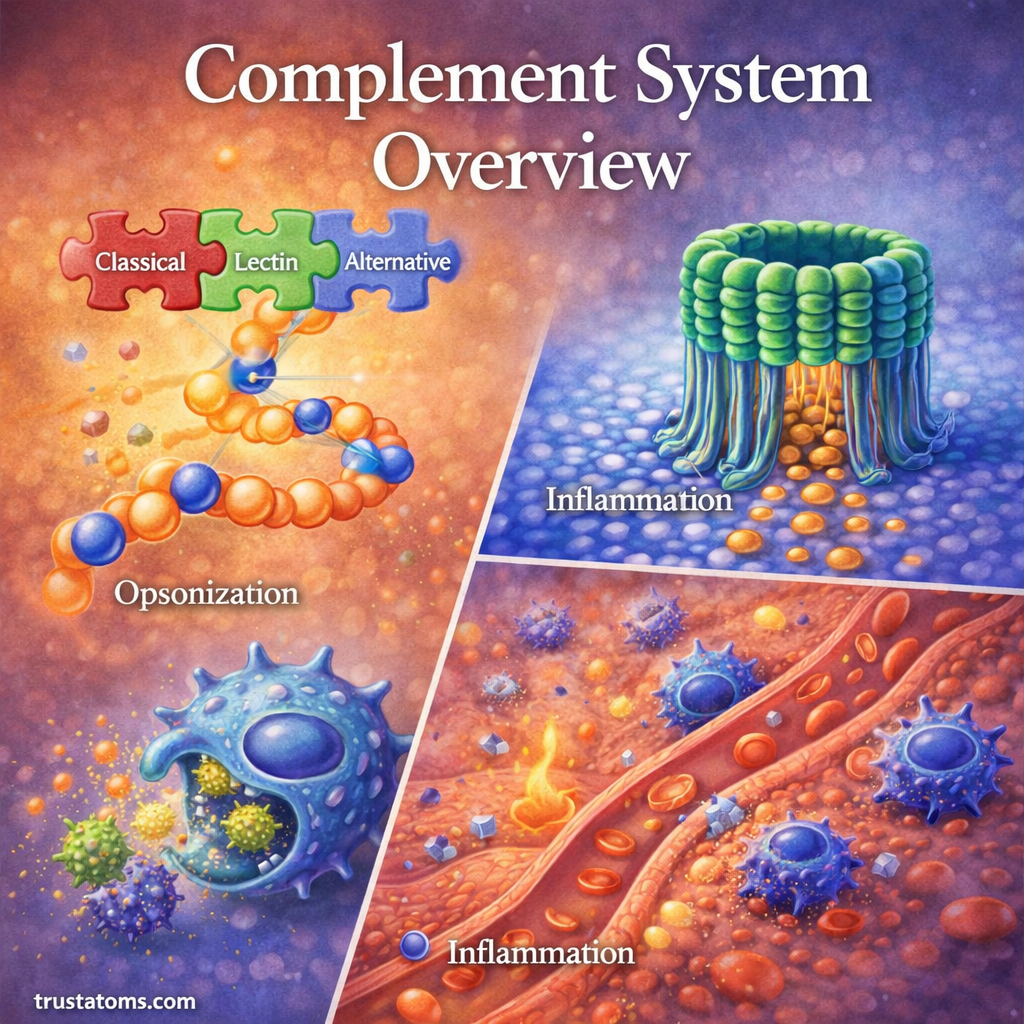
The Three Pathways of Complement Activation
The complement system can be activated through three main pathways. Each pathway is triggered differently, but they all lead to the same outcome.
1. Classical Pathway
- Triggered by antibodies bound to pathogens
- Links closely with adaptive immunity
- Activated when the body recognizes a specific invader
2. Lectin Pathway
- Triggered by proteins binding to sugars on microbial surfaces
- Does not require antibodies
- Part of innate immunity
3. Alternative Pathway
- Activated directly on pathogen surfaces
- Always “on” at a low level
- Provides rapid, non-specific defense
What Happens After Activation?
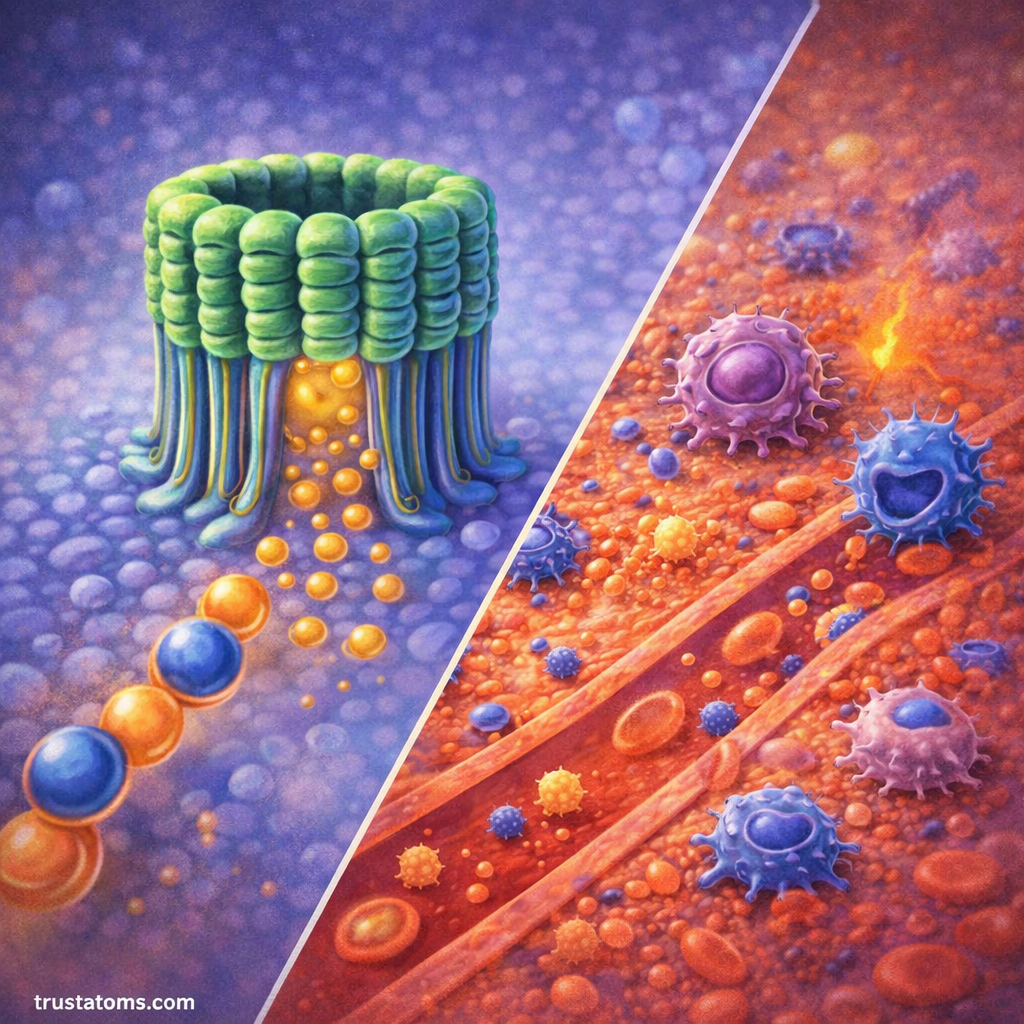
Once activated, the complement system triggers a cascade of reactions. This is often called the complement cascade.
Key Outcomes of Activation
- Opsonization
- Pathogens are coated with complement proteins
- Makes them easier for immune cells to recognize and engulf
- Inflammation
- Signals attract immune cells to the infection site
- Increases blood flow and permeability
- Cell Lysis (Destruction)
- Formation of the membrane attack complex (MAC)
- Creates holes in pathogen membranes
- Leads to cell death
The Membrane Attack Complex (MAC)
One of the most powerful tools of the complement system is the membrane attack complex.
How It Works
- Complement proteins assemble on the pathogen surface
- Form a pore (hole) in the membrane
- Disrupts internal balance
- Causes the pathogen to burst and die
This is especially effective against certain bacteria.
Complement System and Phagocytosis
The complement system works closely with phagocytes.
How They Work Together
- Complement proteins “tag” pathogens
- Phagocytes recognize these tags
- Enhances engulfment and destruction
This process significantly improves the efficiency of immune cells like macrophages and neutrophils.
Regulation of the Complement System
Because the complement system is so powerful, it must be carefully controlled to avoid damaging healthy cells.
Protective Mechanisms
- Regulatory proteins prevent activation on host cells
- Rapid breakdown of active components
- Targeted activation only at infection sites
Without proper regulation, the complement system could harm the body’s own tissues.
Disorders Related to the Complement System
Problems with the complement system can lead to health issues.
Possible Issues
- Increased susceptibility to infections
- Autoimmune conditions (immune system attacking itself)
- Chronic inflammation
These conditions highlight how important balance is within the immune system.
Complement System vs Other Immune Responses
The complement system works alongside other immune defenses but has unique features.
Compared to Innate Immunity
- Faster amplification of response
- Works with existing barriers and cells
Compared to Adaptive Immunity
- Does not require prior exposure
- Enhances antibody effectiveness
How to Support a Healthy Immune System
While the complement system works automatically, overall immune health can influence its effectiveness.
Practical Tips
- Eat a nutrient-rich diet
- Stay hydrated
- Get regular sleep
- Manage stress levels
- Maintain physical activity
Why the Complement System Is Essential
The complement system is a critical part of your body’s defense network. It helps:
- Detect and mark harmful invaders
- Strengthen immune responses
- Destroy pathogens directly
- Coordinate with other immune mechanisms
It ensures that your immune system responds quickly, efficiently, and effectively.
Final Thoughts
The complement system is a powerful and dynamic component of immunity that often works behind the scenes. By amplifying immune responses, tagging pathogens, and directly destroying harmful cells, it plays a vital role in protecting your body.
Understanding how the complement system works gives you a clearer picture of how your immune system stays one step ahead of infection.