Appetite is not simply about hunger—it is a highly regulated biological process controlled by complex interactions between hormones, the brain, and energy stores. The endocrine system plays a central role in signaling when to eat, how much to eat, and when to stop.
This regulation helps maintain energy balance, body weight, and overall metabolic health.
What Is Appetite Regulation?
Appetite regulation refers to the body’s ability to:
- Detect energy needs
- Trigger hunger or fullness
- Adjust food intake accordingly
It involves communication between:
- The digestive system
- Adipose (fat) tissue
- The brain, especially the hypothalamus
- Endocrine glands that release appetite-related hormones
The Hypothalamus: Control Center of Appetite
The hypothalamus is the primary brain region responsible for regulating appetite.
Key Functions
- Receives hormonal signals from the body
- Integrates information about energy status
- Activates hunger or satiety pathways
Two Important Regions
- Lateral hypothalamus → stimulates hunger
- Ventromedial hypothalamus → promotes fullness
This balance ensures the body eats enough to meet energy needs without overconsumption.
Major Hormones That Regulate Appetite
Several hormones work together to control hunger and satiety. These hormones originate from different parts of the body but act on the brain.
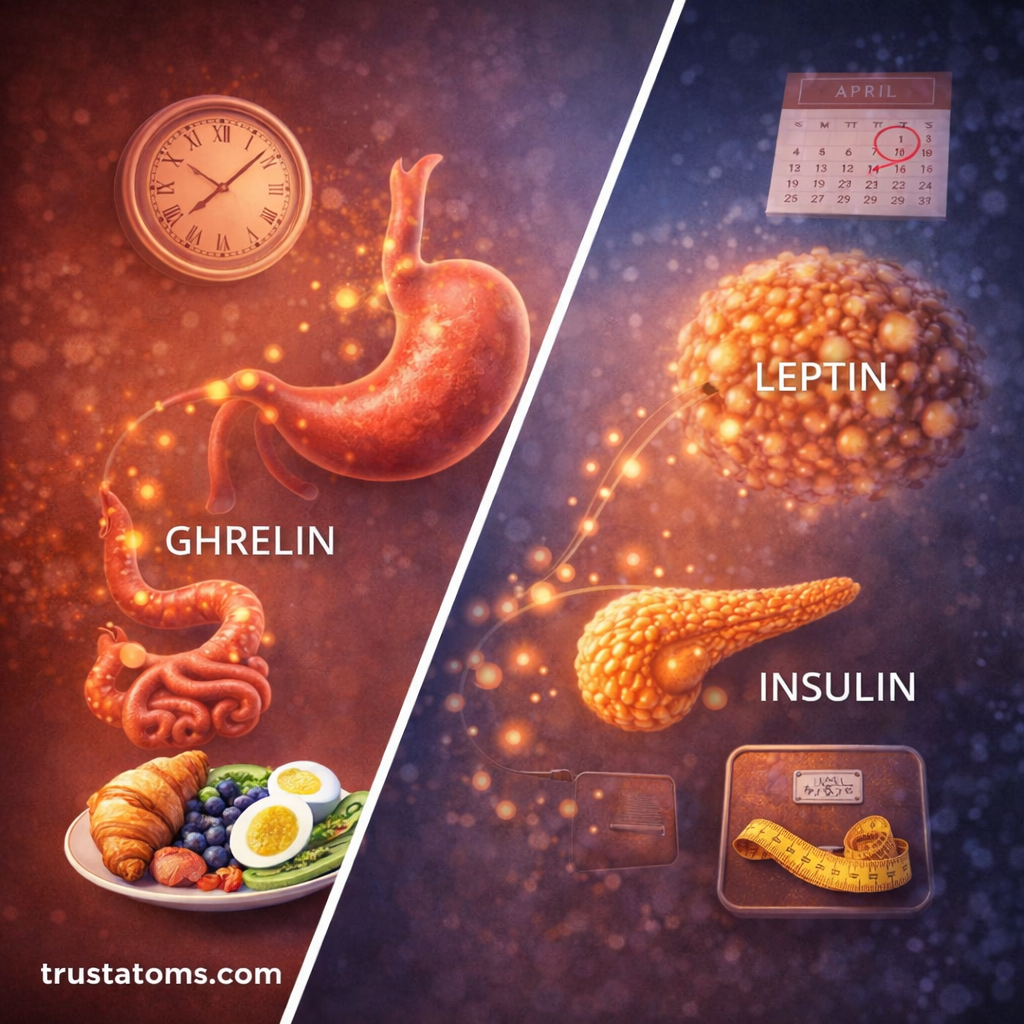
Ghrelin: The Hunger Hormone
- Produced in the stomach
- Levels rise before meals and decrease after eating
Functions:
- Stimulates appetite
- Signals the brain that it’s time to eat
- Promotes food intake
Ghrelin is often called the “hunger hormone” because it directly increases the desire to eat.
Leptin: The Satiety Hormone
- Produced by fat (adipose) tissue
- Reflects long-term energy storage
Functions:
- Suppresses appetite
- Signals the brain that energy stores are sufficient
- Helps regulate body weight
Higher fat stores typically lead to higher leptin levels, reducing hunger—although this system can become dysregulated.
Insulin: Energy Regulation and Appetite
- Released by the pancreas after eating
Functions:
- Helps cells absorb glucose
- Signals satiety to the brain
- Works alongside leptin to reduce food intake
Insulin plays both a metabolic and appetite-regulating role.
Peptide YY (PYY): Short-Term Satiety Signal
- Released by the intestines after meals
Functions:
- Reduces appetite
- Slows digestion
- Signals fullness shortly after eating
PYY helps prevent overeating during a meal.
Cholecystokinin (CCK): Meal-Termination Hormone
- Released by the small intestine in response to food
Functions:
- Promotes feelings of fullness
- Slows gastric emptying
- Signals the brain to stop eating
CCK acts quickly during meals to control portion size.
Short-Term vs Long-Term Regulation
Appetite control operates on two levels:
Short-Term Regulation
- Responds to immediate food intake
- Controlled by gut hormones like:
- Ghrelin
- PYY
- CCK
Purpose:
- Start and stop individual meals
Long-Term Regulation
- Maintains body weight over time
- Controlled by hormones like:
- Leptin
- Insulin
Purpose:
- Adjust overall energy balance
How the Brain Processes Appetite Signals
The hypothalamus integrates signals and activates specific neural pathways.
Two Key Pathways
- Orexigenic Pathway (Stimulates Hunger)
- Activated by ghrelin
- Increases food-seeking behavior
- Anorexigenic Pathway (Suppresses Hunger)
- Activated by leptin, insulin, PYY
- Promotes satiety and reduces intake
These pathways work in opposition to maintain balance.
Feedback Loops in Appetite Regulation
The endocrine system uses feedback mechanisms to fine-tune appetite.
Negative Feedback
- After eating, satiety hormones increase
- Hunger signals decrease
- Prevents excessive food intake
Example Process
- Food is consumed
- Gut releases PYY and CCK
- Insulin levels rise
- Brain receives satiety signals
- Appetite decreases
Factors That Influence Appetite Hormones
Appetite regulation is dynamic and influenced by lifestyle and environmental factors.
Common Influences
- Sleep: Poor sleep increases ghrelin and decreases leptin
- Stress: Chronic stress can elevate cortisol, increasing appetite
- Diet composition: Protein and fiber enhance satiety signals
- Physical activity: Can improve hormonal balance
- Body fat levels: Affect leptin signaling
Disorders of Appetite Regulation
When endocrine signaling is disrupted, appetite control can become impaired.
Common Conditions
- Obesity: Often linked to leptin resistance
- Anorexia nervosa: Altered hunger signaling and perception
- Binge eating disorder: Dysregulated satiety signals
- Diabetes: Insulin dysfunction affects appetite control
Key Takeaways
- Appetite is regulated by hormones, not just willpower
- The hypothalamus is the central control center
- Ghrelin increases hunger, while leptin and insulin promote fullness
- Short-term and long-term systems work together
- Feedback loops prevent overeating and maintain energy balance
- Lifestyle factors strongly influence appetite hormones
Final Thoughts
Endocrine regulation of appetite is essential for maintaining a healthy balance between energy intake and expenditure. By coordinating signals from the stomach, fat tissue, pancreas, and brain, the body ensures that eating behavior aligns with physiological needs.
Understanding these hormonal mechanisms helps explain why appetite can fluctuate—and why maintaining balance involves more than just conscious control.