Pain is one of the body’s most important protective mechanisms. It alerts you to injury, prevents further damage, and drives healing behaviors. But pain is not just a simple sensation—it’s a complex process involving specialized receptors, neural pathways, and brain interpretation.
This guide breaks down how pain works, focusing on nociceptors and the pathways that carry pain signals from the body to the brain.
What Is Pain Perception?
Pain perception refers to how the nervous system detects, transmits, and interprets harmful stimuli. This process involves both the peripheral nervous system and the central nervous system.
There are two key components:
- Detection of a harmful stimulus (like heat, pressure, or chemicals)
- Interpretation of that signal as “pain” in the brain
Pain is subjective, meaning two people can experience the same injury very differently depending on biological and psychological factors.
What Are Nociceptors?
Nociceptors are specialized sensory receptors that detect potentially damaging stimuli. They are free nerve endings found in:
- Skin
- Muscles
- Joints
- Internal organs
Unlike other sensory receptors, nociceptors do not adapt easily. This means they continue to fire as long as the harmful stimulus is present.
Types of Nociceptors
Nociceptors can be classified based on the type of stimulus they detect:
- Mechanical nociceptors
Respond to strong pressure or physical damage (e.g., cuts or impacts) - Thermal nociceptors
Activated by extreme heat or cold - Chemical nociceptors
Triggered by substances released during tissue damage (e.g., prostaglandins, bradykinin) - Polymodal nociceptors
Respond to multiple types of stimuli (mechanical, thermal, and chemical)
Types of Pain
Pain can be categorized based on its source and duration.
Based on Source
- Somatic pain
Originates from skin, muscles, or joints (sharp, localized) - Visceral pain
Comes from internal organs (dull, diffuse, often hard to pinpoint) - Referred pain
Pain felt in a different location than the source (e.g., arm pain during a heart attack)
Based on Duration
- Acute pain
Short-term, usually linked to injury or illness - Chronic pain
Lasts longer than 3 months and may persist after healing
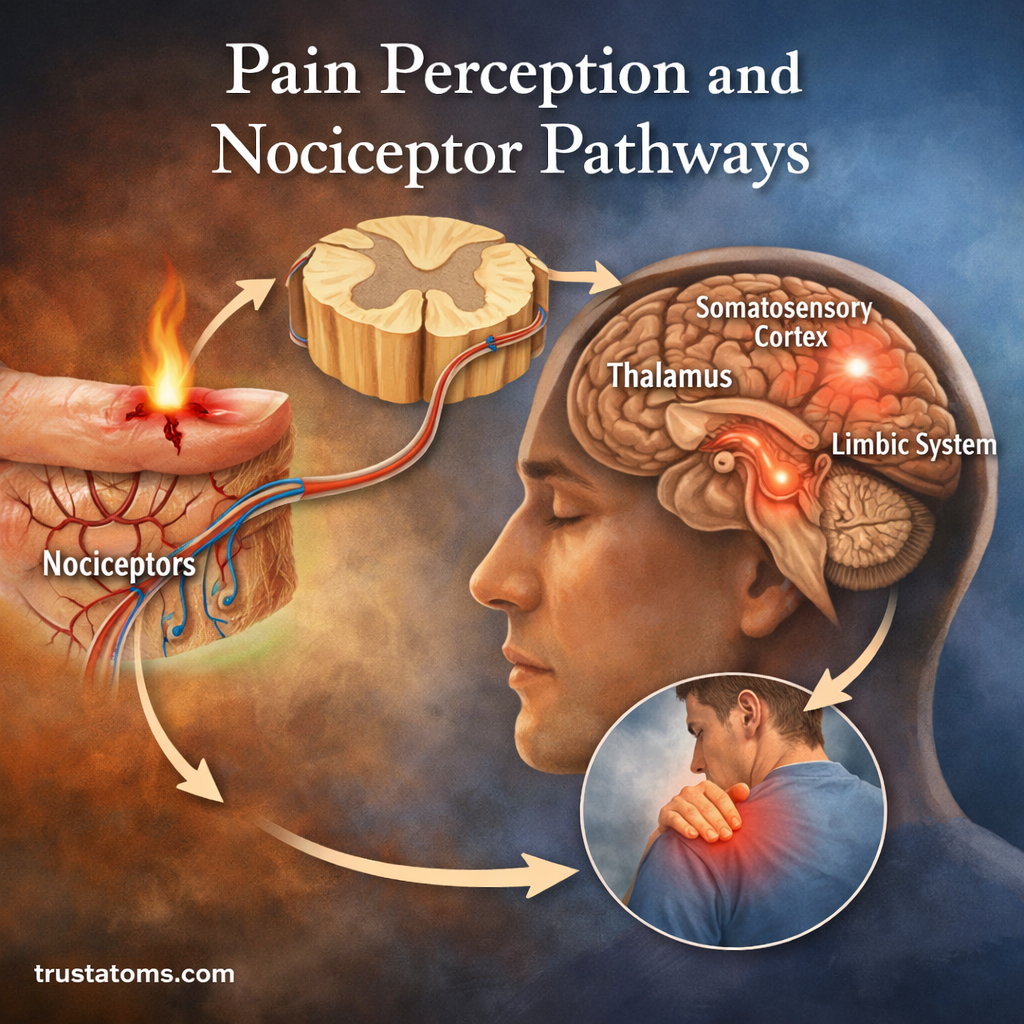
The Pain Pathway: Step-by-Step
Pain perception follows a structured pathway from the site of injury to the brain. This is often described in four stages.
1. Transduction
This is the process of converting a harmful stimulus into an electrical signal.
- Tissue damage releases chemicals (like prostaglandins)
- Nociceptors detect these changes
- Electrical impulses are generated in the sensory neurons
2. Transmission
The pain signal travels from the site of injury to the spinal cord and brain.
Key steps include:
- Signal travels along peripheral nerves via A-delta and C fibers
- A-delta fibers: fast, sharp pain
- C fibers: slow, dull pain
- Signal enters the spinal cord through the dorsal horn
- Neurons relay the signal upward through the spinal cord to the brain
3. Perception
Pain is consciously experienced in the brain.
Major brain regions involved:
- Thalamus (relay center)
- Somatosensory cortex (location and intensity)
- Limbic system (emotional response)
This is where pain becomes a subjective experience.
4. Modulation
The body can increase or decrease pain signals through modulation.
- Descending pathways from the brain can inhibit pain signals
- Neurotransmitters like endorphins reduce pain perception
- This explains why pain can feel less intense during stress or distraction
Key Neural Pathways in Pain Transmission
Pain signals travel through specific neural tracts in the spinal cord.
Spinothalamic Tract
The primary pathway for pain and temperature signals.
- Carries signals from the spinal cord to the thalamus
- Allows the brain to identify the location and intensity of pain
Other Important Pathways
- Spinoreticular tract
Involved in emotional and alertness aspects of pain - Spinomesencephalic tract
Plays a role in pain modulation and reflex responses
Fast vs Slow Pain
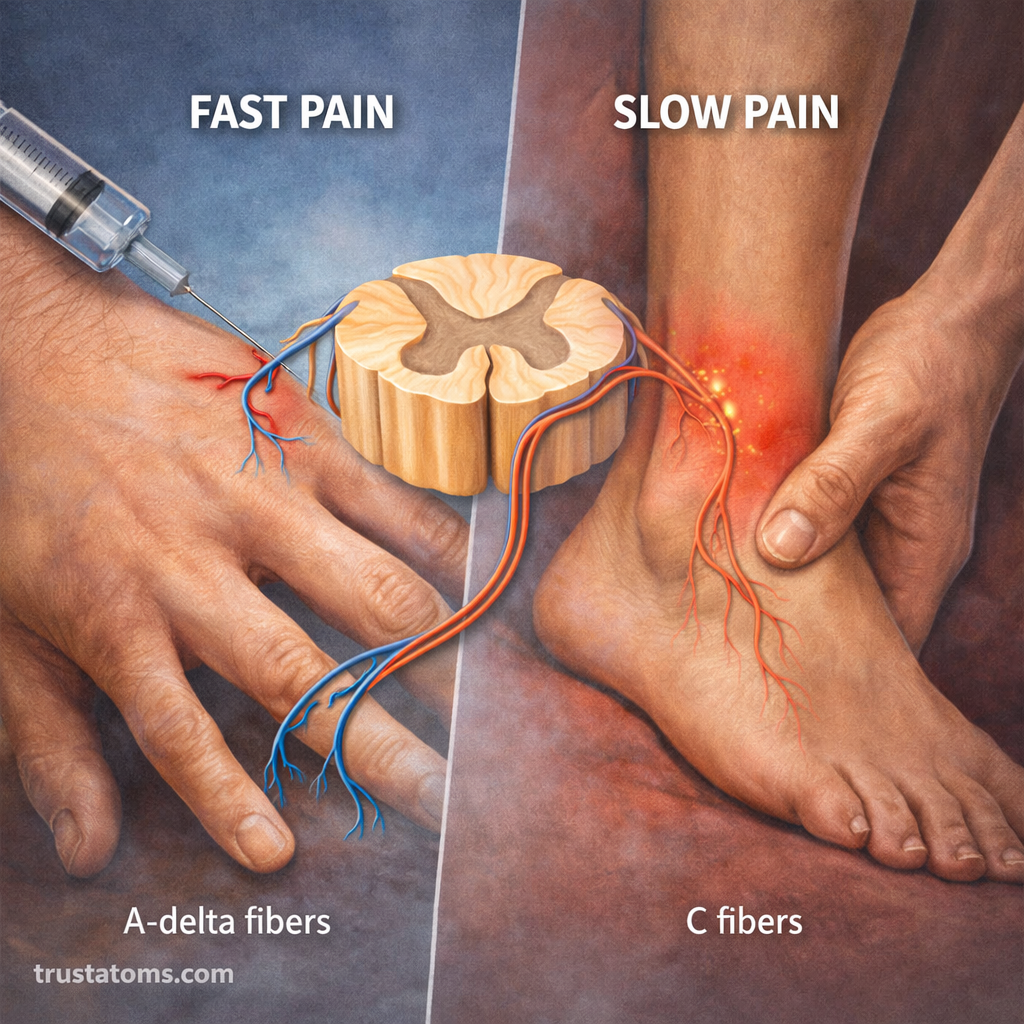
Pain is often experienced in two phases due to different nerve fibers.
Fast Pain
- Carried by A-delta fibers
- Sharp, well-localized
- Felt immediately after injury
Slow Pain
- Carried by C fibers
- Dull, aching, or burning
- Develops more gradually
This is why a sharp pain from a cut may be followed by a lingering ache.
Factors That Influence Pain Perception
Pain is not purely physical—it is influenced by multiple factors.
Biological Factors
- Injury severity
- Inflammation
- Nervous system sensitivity
Psychological Factors
- Attention and focus
- Stress or anxiety
- Past experiences
Social and Environmental Factors
- Cultural expectations
- Support systems
- Context of the injury
These factors explain why pain experiences vary widely between individuals.
Clinical Relevance
Understanding pain pathways is essential in medicine and healthcare.
Pain Management Approaches
- Medications
- NSAIDs reduce inflammation
- Opioids affect central pain pathways
- Physical therapy
Helps restore function and reduce pain signals - Cognitive strategies
Techniques like mindfulness can alter pain perception
Common Disorders Related to Pain Pathways
Disruptions in nociceptor function or neural pathways can lead to abnormal pain.
- Neuropathic pain
Caused by nerve damage (e.g., diabetic neuropathy) - Hyperalgesia
Increased sensitivity to pain - Allodynia
Pain from stimuli that are normally not painful
These conditions highlight how complex and sensitive the pain system is.
Final Thoughts
Pain perception is a multi-step process involving detection, transmission, interpretation, and modulation. Nociceptors serve as the body’s early warning system, while complex neural pathways ensure that signals reach the brain for processing.
Understanding how pain works not only explains everyday experiences like injury and recovery but also provides insight into medical treatments and chronic pain conditions.