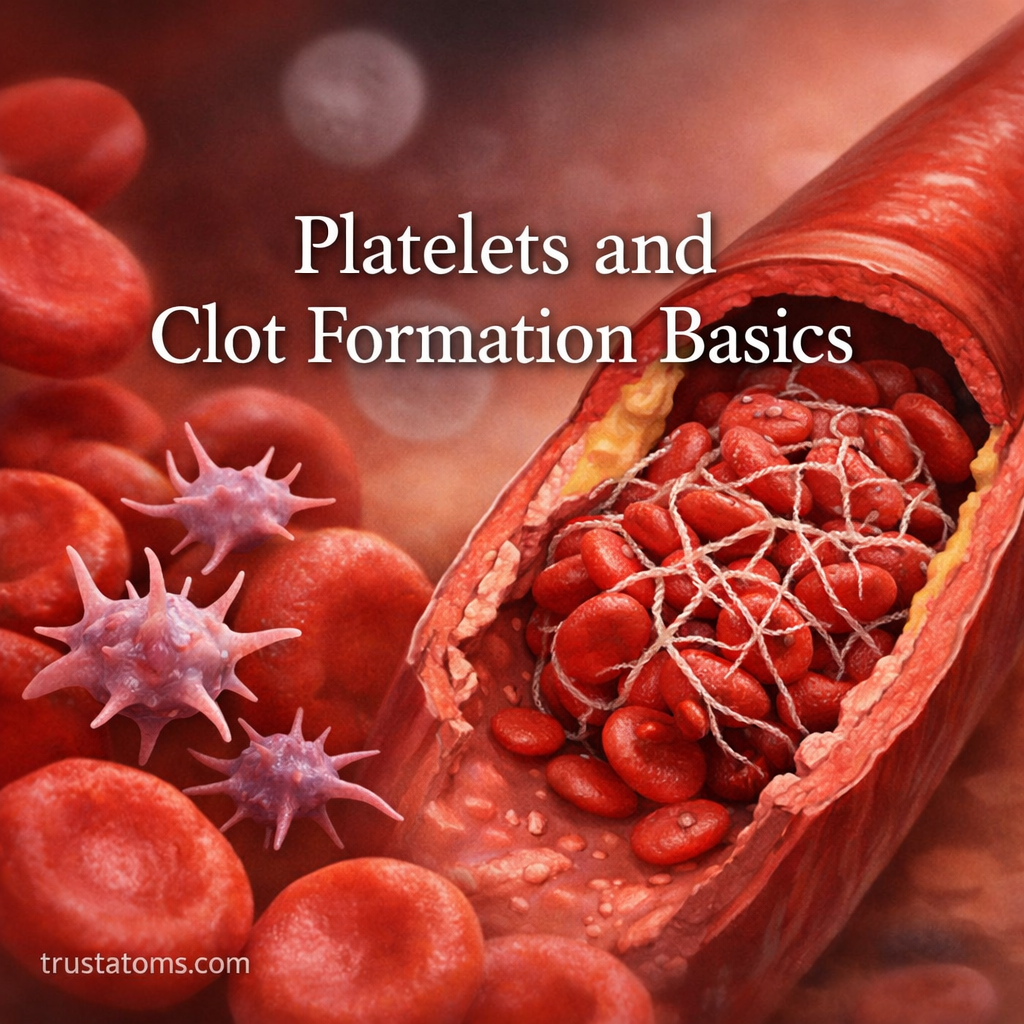
When you get a cut or injury, your body reacts almost instantly to stop the bleeding. This life-saving process is called clot formation (or coagulation), and platelets play a central role. Despite being tiny and often overlooked, platelets are essential for preventing excessive blood loss and supporting healing.
In this guide, you’ll learn what platelets are, how clot formation works step by step, and why this process is so important for your health.
What Are Platelets?
Platelets, also known as thrombocytes, are small, colorless cell fragments found in your blood. Unlike red or white blood cells, platelets are not complete cells—they are pieces of larger cells formed in the bone marrow.
Key characteristics of platelets:
- Produced in the bone marrow from megakaryocytes
- Circulate in the blood for about 7–10 days
- Lack a nucleus (making them cell fragments, not full cells)
- Contain proteins and chemicals needed for clotting
Their main job is simple but critical: stop bleeding by forming clots.
Why Clot Formation Is Important
Clot formation is your body’s natural defense against blood loss. Without it, even minor injuries could lead to serious complications.
Clotting helps to:
- Prevent excessive bleeding
- Protect against infection by sealing wounds
- Start the healing process
- Maintain stable blood circulation
This process is tightly controlled—too little clotting leads to bleeding disorders, while too much can cause dangerous blockages.
The Step-by-Step Process of Clot Formation
Clot formation (hemostasis) occurs in a series of coordinated steps. Each step builds on the previous one to quickly stop bleeding.
1. Blood Vessel Constriction (Vasoconstriction)
When a blood vessel is damaged, it immediately narrows.
- Reduces blood flow to the injured area
- Limits blood loss
- Buys time for platelets to respond
This is the body’s first rapid reaction.
2. Platelet Adhesion
Platelets quickly move to the site of injury and stick to the exposed surface of the damaged vessel.
- They bind to collagen fibers exposed by injury
- Specialized proteins help them attach securely
- This creates the foundation for a clot
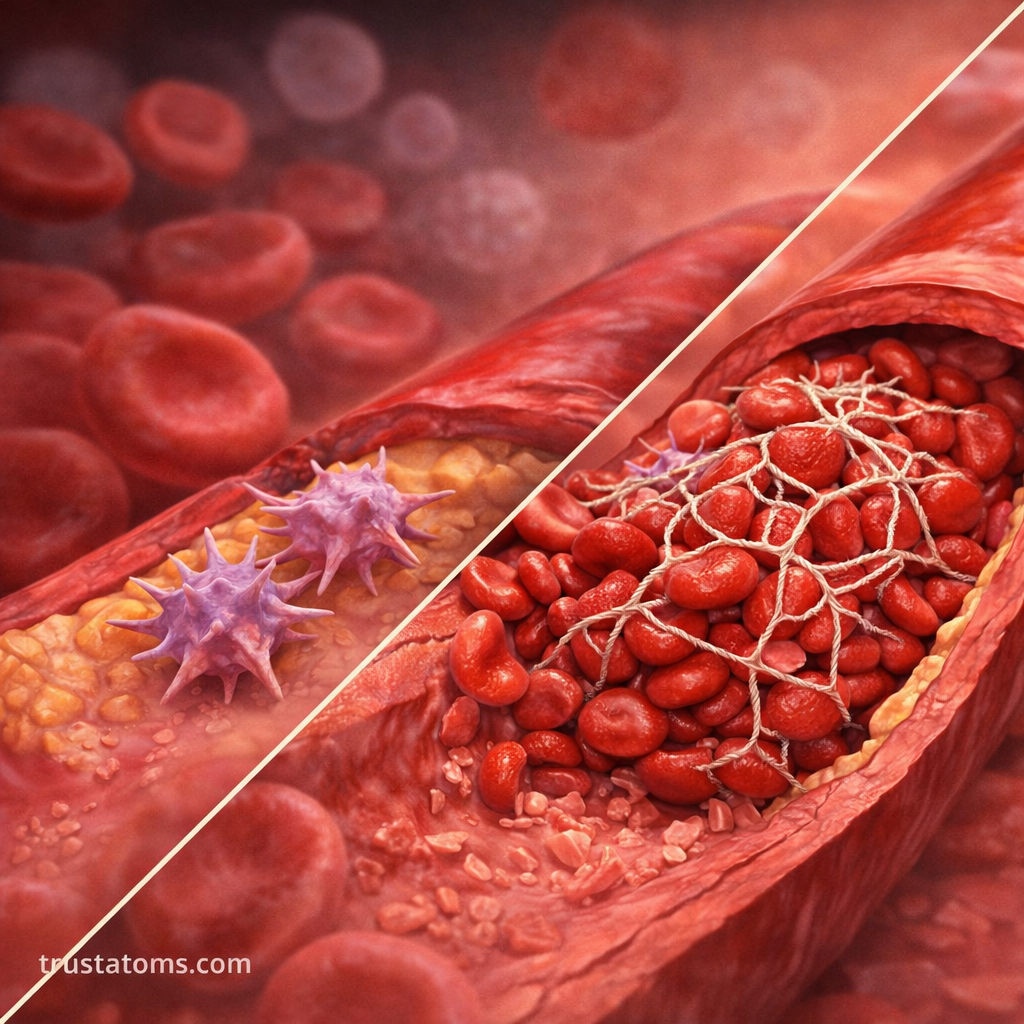
3. Platelet Activation
Once platelets stick to the injury site, they become activated.
- They change shape (becoming spiky and sticky)
- Release chemical signals (like ADP and thromboxane)
- Attract more platelets to the area
This creates a positive feedback loop, rapidly increasing platelet activity.
4. Platelet Aggregation (Platelet Plug Formation)
Activated platelets begin to clump together.
- Form a temporary “platelet plug”
- Quickly seals small breaks in blood vessels
- Acts as a scaffold for the next step
This plug alone may be enough for minor injuries.
5. Coagulation (Fibrin Clot Formation)
For stronger, long-lasting repair, the body reinforces the platelet plug.
- A cascade of clotting factors activates proteins in the blood
- Fibrin (a strong, thread-like protein) is produced
- Fibrin forms a mesh over the platelet plug
This mesh stabilizes the clot and prevents it from breaking apart.
6. Clot Retraction and Healing
After the clot forms:
- Platelets contract to tighten the clot
- Edges of the wound are pulled closer together
- Tissue repair begins
Eventually, the clot dissolves once healing is complete.
Key Components Involved in Clotting
Clot formation relies on several important elements working together.
Platelets
- Form the initial plug
- Release signaling chemicals
Clotting Factors
- Proteins in the blood that activate in sequence
- Lead to fibrin formation
Fibrin
- Creates a strong mesh
- Stabilizes the clot
Calcium and Vitamin K
- Essential for activating clotting factors
- Help regulate the clotting process
What Happens When Clotting Goes Wrong?
The clotting system must stay balanced. Problems can occur when it becomes too weak or too active.
Too little clotting (bleeding disorders):
- Easy bruising
- Prolonged bleeding
- Conditions like hemophilia
Too much clotting (thrombosis):
- Blood clots forming inside vessels
- Can lead to heart attack or stroke
- Conditions like deep vein thrombosis (DVT)
Maintaining this balance is critical for overall health.
How Platelets Support Healing
Beyond stopping bleeding, platelets also play a role in recovery.
- Release growth factors that promote tissue repair
- Help rebuild damaged blood vessels
- Support immune responses at injury sites
This makes platelets essential not just for protection—but for healing and regeneration.
Final Thoughts
Platelets and clot formation are vital to survival. From the moment a blood vessel is damaged, a rapid and highly coordinated process begins to prevent blood loss and initiate healing.
Understanding how this system works highlights just how efficient and complex the human body is. Even the smallest components—like platelets—play a powerful role in keeping you safe and healthy.