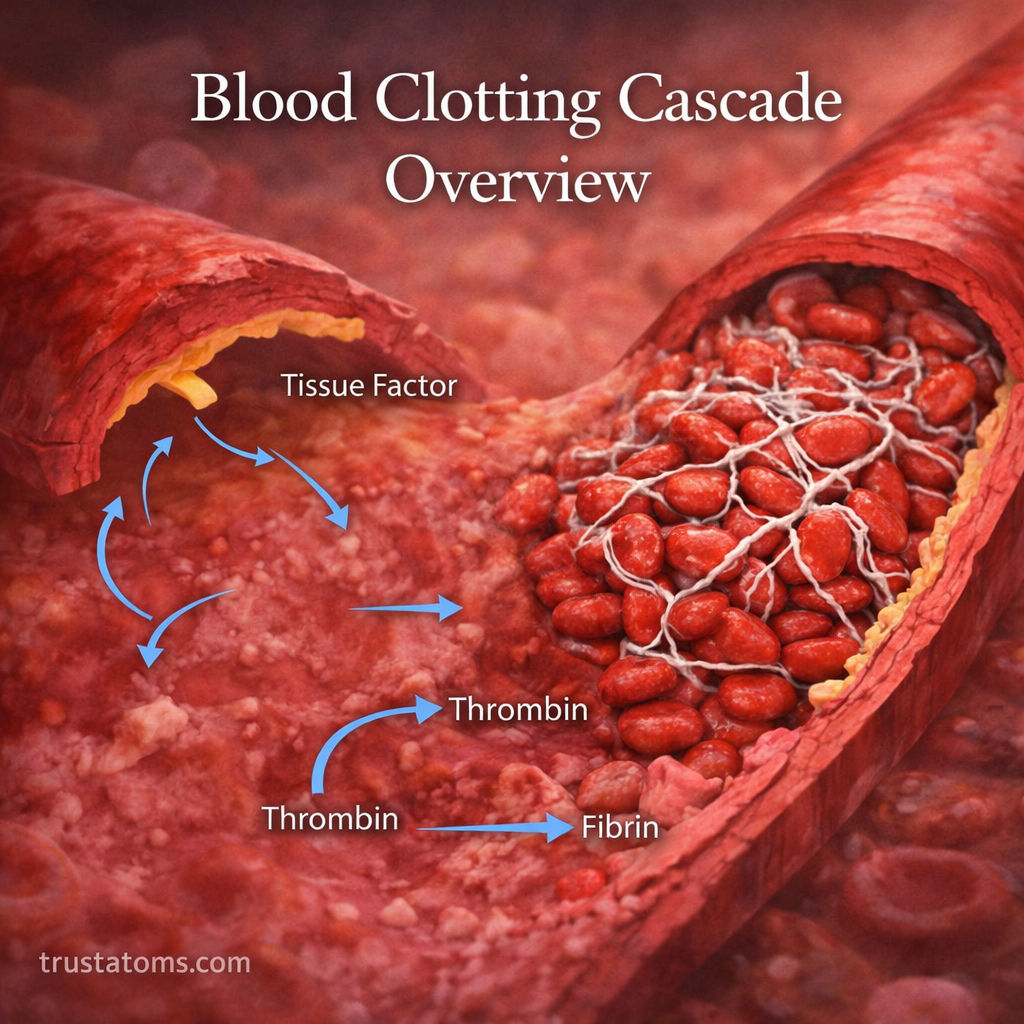
The human body has a remarkable ability to stop bleeding quickly after injury. This process relies on a complex chain reaction known as the blood clotting cascade. While platelets form the initial plug, the clotting cascade strengthens and stabilizes it, ensuring long-term protection and proper healing.
In this guide, you’ll learn how the clotting cascade works, the key pathways involved, and why this system is essential for survival.
What Is the Blood Clotting Cascade?
The blood clotting cascade is a series of chemical reactions involving clotting factors—special proteins found in your blood.
Each factor activates the next in a step-by-step sequence, similar to a domino effect. This leads to the formation of fibrin, a strong protein that stabilizes blood clots.
Key features of the cascade:
- Involves multiple clotting factors (labeled I to XIII)
- Occurs rapidly after vessel injury
- Amplifies signals for efficient clot formation
- Ends with a stable fibrin clot
Why the Clotting Cascade Matters
Without the clotting cascade, the body would not be able to form strong, lasting clots.
Its main functions include:
- Reinforcing the platelet plug
- Preventing continued blood loss
- Supporting wound healing
- Maintaining circulatory stability
A properly functioning cascade is essential—imbalances can lead to bleeding disorders or dangerous clots.
The Three Main Pathways of the Clotting Cascade
The clotting cascade is divided into three interconnected pathways:
- Intrinsic pathway
- Extrinsic pathway
- Common pathway
Each pathway plays a specific role in forming a clot.
Intrinsic Pathway (Contact Activation Pathway)
The intrinsic pathway is triggered by damage inside the blood vessel.
What activates it:
- Exposure of blood to collagen
- Internal vessel injury
- Contact with abnormal surfaces
Key characteristics:
- Involves clotting factors XII, XI, IX, and VIII
- Slower than the extrinsic pathway
- Amplifies clotting signals
This pathway strengthens and sustains clot formation over time.
Extrinsic Pathway (Tissue Factor Pathway)
The extrinsic pathway is activated by external trauma that causes blood to escape from the vessel.
What activates it:
- Tissue damage outside the vessel
- Release of tissue factor (Factor III)
Key characteristics:
- Involves Factor VII and tissue factor
- Faster than the intrinsic pathway
- Acts as the initial trigger for clotting
This pathway quickly starts the clotting process after injury.
Common Pathway
Both the intrinsic and extrinsic pathways merge into the common pathway, which produces the final clot.
Key steps in the common pathway:
- Activation of Factor X
- Conversion of prothrombin (Factor II) into thrombin
- Conversion of fibrinogen (Factor I) into fibrin
- Formation of a stable fibrin mesh
This fibrin mesh acts like a net, trapping blood cells and strengthening the clot.
Role of Thrombin in Clot Formation
Thrombin is one of the most important enzymes in the clotting cascade.
Functions of thrombin:
- Converts fibrinogen into fibrin
- Activates additional clotting factors
- Strengthens the clotting response
- Enhances platelet activation
Thrombin essentially accelerates and amplifies the entire process.
Key Clotting Factors to Know
Clotting factors are proteins that circulate in an inactive form until needed.
Important examples:
- Factor I – Fibrinogen
- Factor II – Prothrombin
- Factor III – Tissue factor
- Factor V – Accelerator protein
- Factor VIII – Anti-hemophilic factor
- Factor X – Central to the common pathway
Most clotting factors are produced in the liver and require vitamin K for proper function.
Step-by-Step Summary of the Cascade
To simplify, here’s how the clotting cascade unfolds:
- Injury triggers intrinsic and/or extrinsic pathways
- Clotting factors activate in sequence
- Factor X is activated
- Thrombin is produced
- Fibrin forms a mesh
- A stable clot develops
This sequence ensures fast and effective bleeding control.
How the Body Regulates Clotting
The clotting system must remain balanced to prevent problems.
The body uses several controls:
- Anticoagulants (e.g., antithrombin) to slow clotting
- Fibrinolysis to break down clots after healing
- Endothelial cells to regulate clot formation
These mechanisms prevent excessive clotting while still allowing protection.
What Happens When the Cascade Malfunctions?
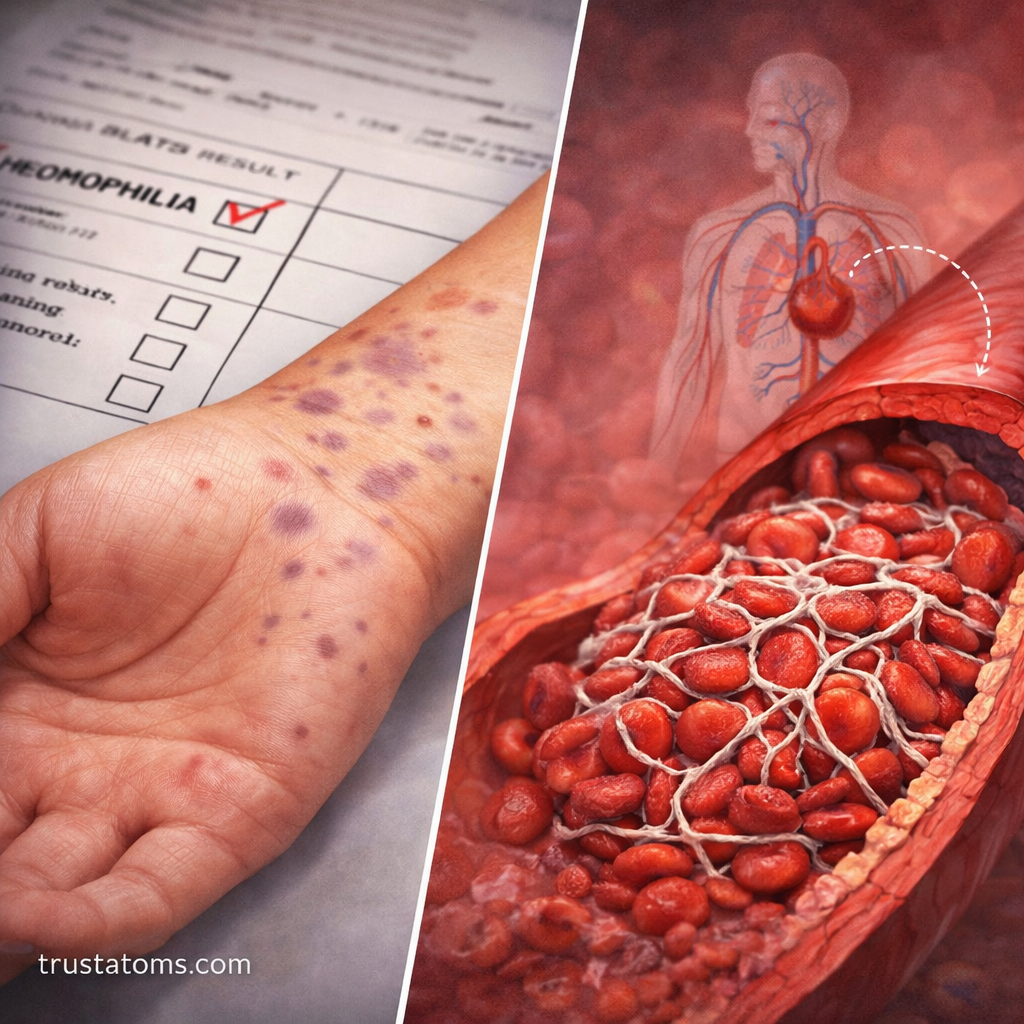
Problems in the clotting cascade can lead to serious health conditions.
Bleeding disorders:
- Hemophilia (deficiency in Factor VIII or IX)
- Excessive bleeding after injury
- Easy bruising
Clotting disorders:
- Deep vein thrombosis (DVT)
- Pulmonary embolism
- Increased risk of stroke or heart attack
Maintaining proper function is essential for overall health.
Final Thoughts
The blood clotting cascade is a finely tuned system that protects the body from blood loss while supporting healing. Through a coordinated series of reactions, clotting factors work together to create strong, stable clots when needed.
Understanding this process not only highlights the complexity of human biology but also helps explain many medical conditions related to bleeding and clotting.