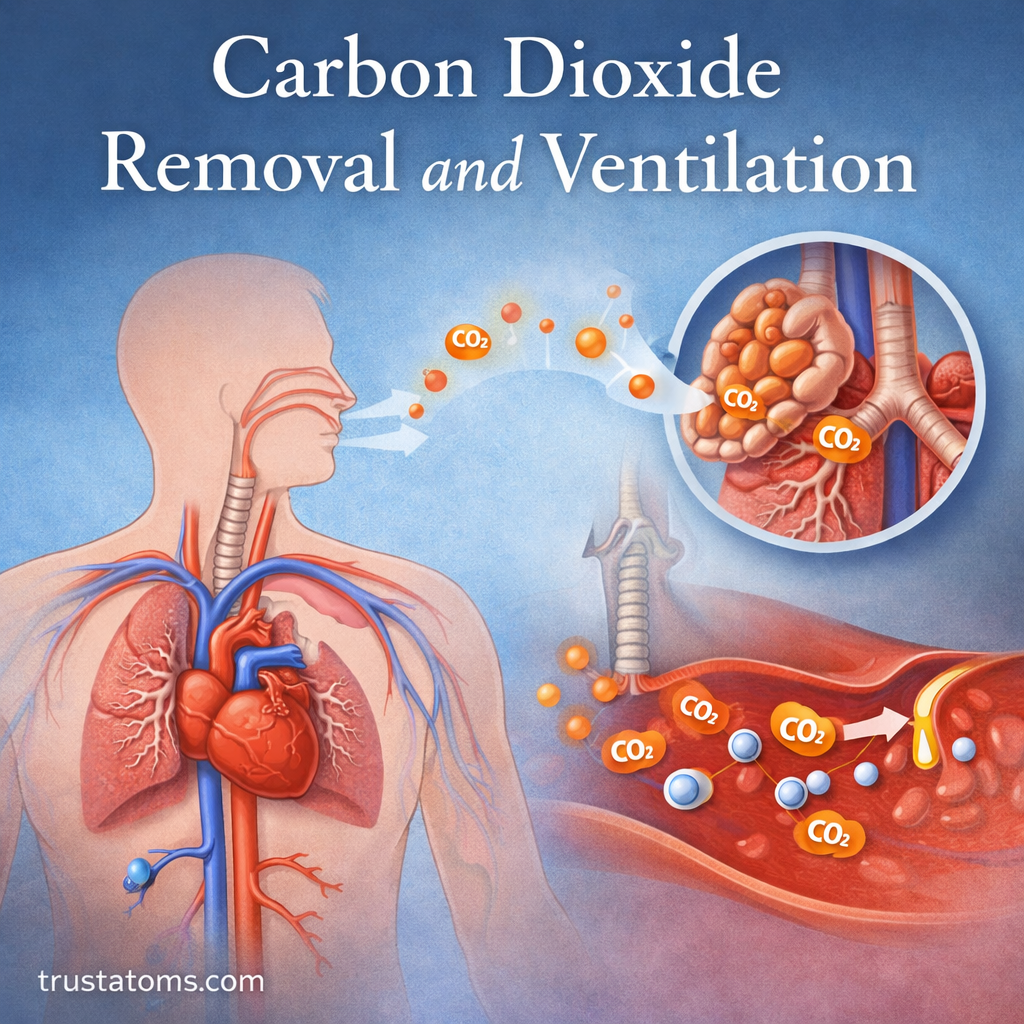
Carbon dioxide (CO₂) removal is just as important as oxygen delivery in maintaining a stable internal environment. Every time your cells produce energy, they generate carbon dioxide as a waste product. If this gas is not efficiently removed, it can disrupt blood pH and impair normal body function.
Ventilation—the process of breathing—plays a central role in clearing carbon dioxide from the body and maintaining balance.
Overview of Carbon Dioxide Removal
Carbon dioxide removal involves three major steps:
- Production in body tissues
- Transport through the bloodstream
- Elimination through the lungs
Each step is tightly regulated to keep blood chemistry within a narrow, healthy range.
Step 1: Carbon Dioxide Is Produced in Cells
Carbon dioxide is generated during cellular respiration, the process cells use to produce energy (ATP).
Where CO₂ Comes From
- Produced in mitochondria during metabolism
- Generated as a byproduct of breaking down nutrients
- Continuously formed in all active tissues
The more active your body is, the more carbon dioxide your cells produce.
Step 2: Carbon Dioxide Enters the Bloodstream
Once produced, carbon dioxide diffuses from cells into nearby capillaries.
Why Diffusion Occurs
- Higher CO₂ concentration in tissues than in blood
- Gas moves from high to low concentration
- Thin capillary walls allow rapid exchange
This movement ensures carbon dioxide is quickly removed from tissues.
Step 3: Carbon Dioxide Transport in Blood
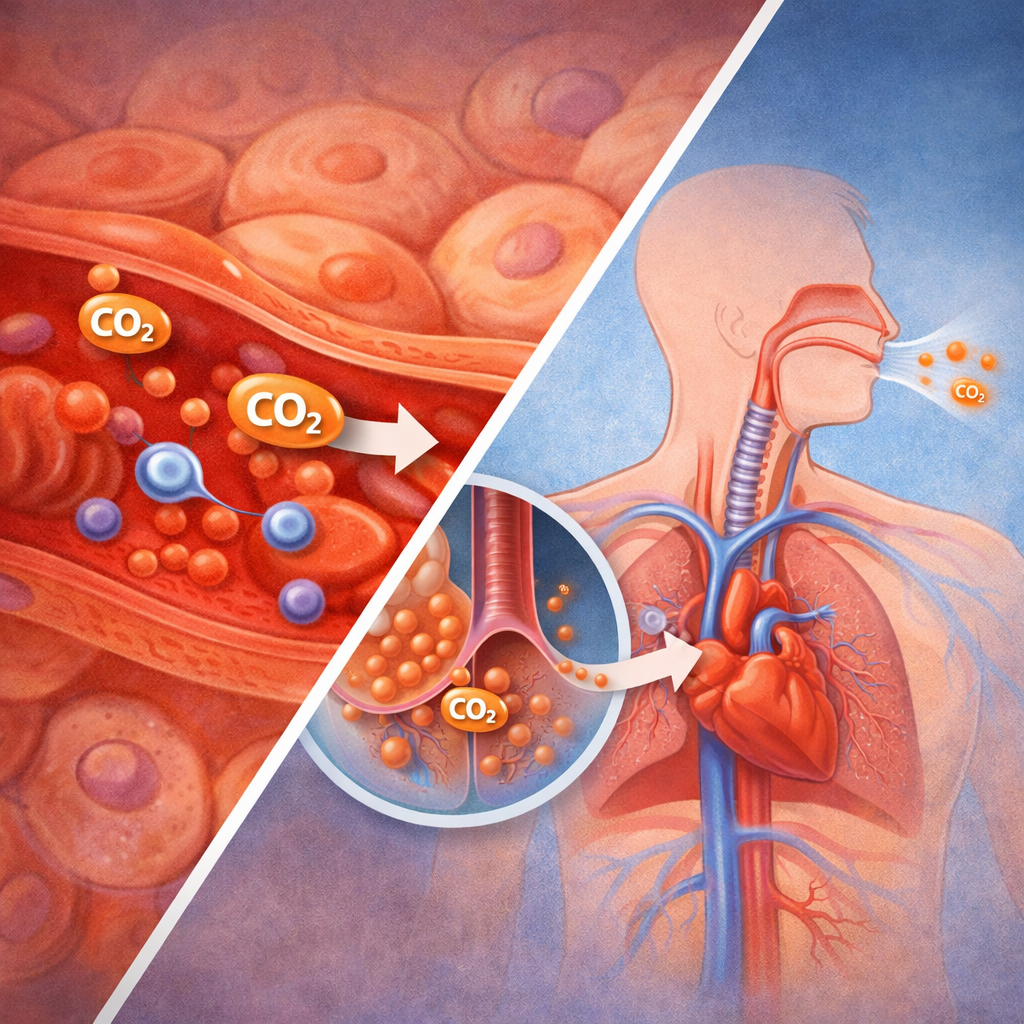
Carbon dioxide travels through the bloodstream in three primary forms:
1. Dissolved in Plasma (~7%)
- CO₂ is directly carried in liquid form
- Contributes to blood acidity
2. Bound to Hemoglobin (~23%)
- Attaches to proteins in red blood cells
- Forms carbaminohemoglobin
3. Converted to Bicarbonate (~70%)
- The majority of CO₂ is converted into bicarbonate ions (HCO₃⁻)
- Occurs inside red blood cells with the help of enzymes
This conversion is crucial for maintaining acid-base balance in the body.
Step 4: Carbon Dioxide Returns to the Lungs
Carbon dioxide-rich blood travels back to the lungs through the circulatory system.
Pathway Back to the Lungs
- Tissues → Venules → Veins
- Right atrium of the heart
- Right ventricle
- Pulmonary arteries
- Lungs
Once in the lungs, carbon dioxide is ready to be expelled.
Step 5: Carbon Dioxide Is Exhaled
In the lungs, carbon dioxide moves from the blood into the alveoli and is removed during exhalation.
How CO₂ Leaves the Body
- Diffuses from blood into alveoli
- Moves down a concentration gradient
- Expelled when you breathe out
This process completes the cycle of gas exchange.
The Role of Ventilation
Ventilation refers to the mechanical process of breathing—inhaling oxygen and exhaling carbon dioxide.
Key Components of Ventilation
- Diaphragm contraction pulls air into the lungs
- Chest cavity expands, lowering internal pressure
- Air flows into the lungs (inhalation)
- Relaxation pushes air out (exhalation)
Ventilation ensures fresh air reaches the alveoli and waste gases are removed.
How Breathing Is Controlled
The body automatically regulates breathing to match carbon dioxide levels.
Primary Control Mechanisms
- Chemoreceptors detect CO₂ levels in blood
- Increased CO₂ triggers faster, deeper breathing
- Decreased CO₂ slows breathing rate
This system keeps blood pH stable and prevents dangerous imbalances.
Carbon Dioxide and Blood pH
Carbon dioxide plays a major role in regulating the acidity of the blood.
The CO₂–pH Relationship
- CO₂ combines with water to form carbonic acid
- Carbonic acid lowers blood pH
- Increased CO₂ → more acidic blood
- Decreased CO₂ → more alkaline blood
Maintaining this balance is essential for enzyme function and overall health.
Factors That Affect CO₂ Removal
Several conditions can influence how effectively carbon dioxide is removed:
1. Lung Function
- Healthy lungs improve gas exchange
- Diseases like COPD reduce efficiency
2. Breathing Rate
- Faster breathing removes more CO₂
- Slower breathing may cause CO₂ buildup
3. Blood Flow
- Efficient circulation transports CO₂ quickly
- Poor circulation slows removal
4. Physical Activity
- Exercise increases CO₂ production
- Ventilation increases to compensate
Common Disorders Affecting CO₂ Removal
Disruptions in carbon dioxide removal can lead to serious health issues.
Examples Include:
- Respiratory acidosis: Excess CO₂ lowers blood pH
- Hyperventilation: Too much CO₂ is removed, raising pH
- Chronic lung diseases: Impaired gas exchange
- Neurological conditions: Disrupted breathing control
These conditions highlight the importance of proper ventilation and gas exchange.
Why Carbon Dioxide Removal Matters
Efficient CO₂ removal is essential for:
- Maintaining stable blood pH
- Preventing toxic buildup of waste gases
- Supporting normal brain and organ function
- Enabling physical activity and endurance
Even small imbalances can affect how your body performs and feels.
Final Thoughts
Carbon dioxide removal and ventilation are critical processes that work continuously to maintain internal balance. From cellular production to exhalation, every step is carefully regulated to keep your body functioning efficiently.
By understanding how CO₂ is transported and eliminated, you gain insight into the importance of healthy lungs, proper breathing, and overall respiratory function.