High-altitude environments present a unique challenge to the human body. As elevation increases, atmospheric pressure drops, meaning less oxygen is available with each breath. Despite this, millions of people live, work, and even perform intense physical activity at high altitudes.
So how does the body adapt?
This article explores the fascinating respiratory changes that occur when humans are exposed to high-altitude conditions—whether for a short trip or long-term living.
What Happens to Oxygen at High Altitude?
At sea level, oxygen is abundant and easily transferred from the lungs into the bloodstream. However, as altitude increases:
- Barometric pressure decreases
- Oxygen partial pressure drops
- Less oxygen enters the lungs with each breath
This condition is known as hypobaric hypoxia.
As a result, the body must compensate quickly to maintain adequate oxygen delivery to tissues.
Immediate Respiratory Responses
When you first arrive at high altitude, your body reacts within minutes.
Increased Breathing Rate (Hyperventilation)
One of the earliest responses is an increase in breathing rate, known as hyperventilation.
This helps:
- Bring more oxygen into the lungs
- Increase oxygen concentration in the blood
- Compensate for reduced oxygen availability
However, this rapid breathing also causes more carbon dioxide (CO₂) to be exhaled, which can disrupt the body’s pH balance.
Respiratory Alkalosis
As CO₂ levels drop, blood becomes more alkaline—a condition called respiratory alkalosis.
Short-term effects may include:
- Lightheadedness
- Tingling sensations
- Mild dizziness
Over time, the body adjusts to restore balance.
Short-Term Adaptations (Days to Weeks)
If you remain at high altitude for several days, your body begins to make more structured adjustments.
Increased Lung Ventilation Efficiency
Your breathing becomes:
- Deeper
- More efficient
- Better coordinated
This improves oxygen uptake without excessive energy expenditure.
Kidney Compensation
To counteract respiratory alkalosis, the kidneys:
- Excrete bicarbonate
- Help normalize blood pH
This allows sustained higher breathing rates without discomfort.
Long-Term Respiratory Adaptations (Weeks to Months)
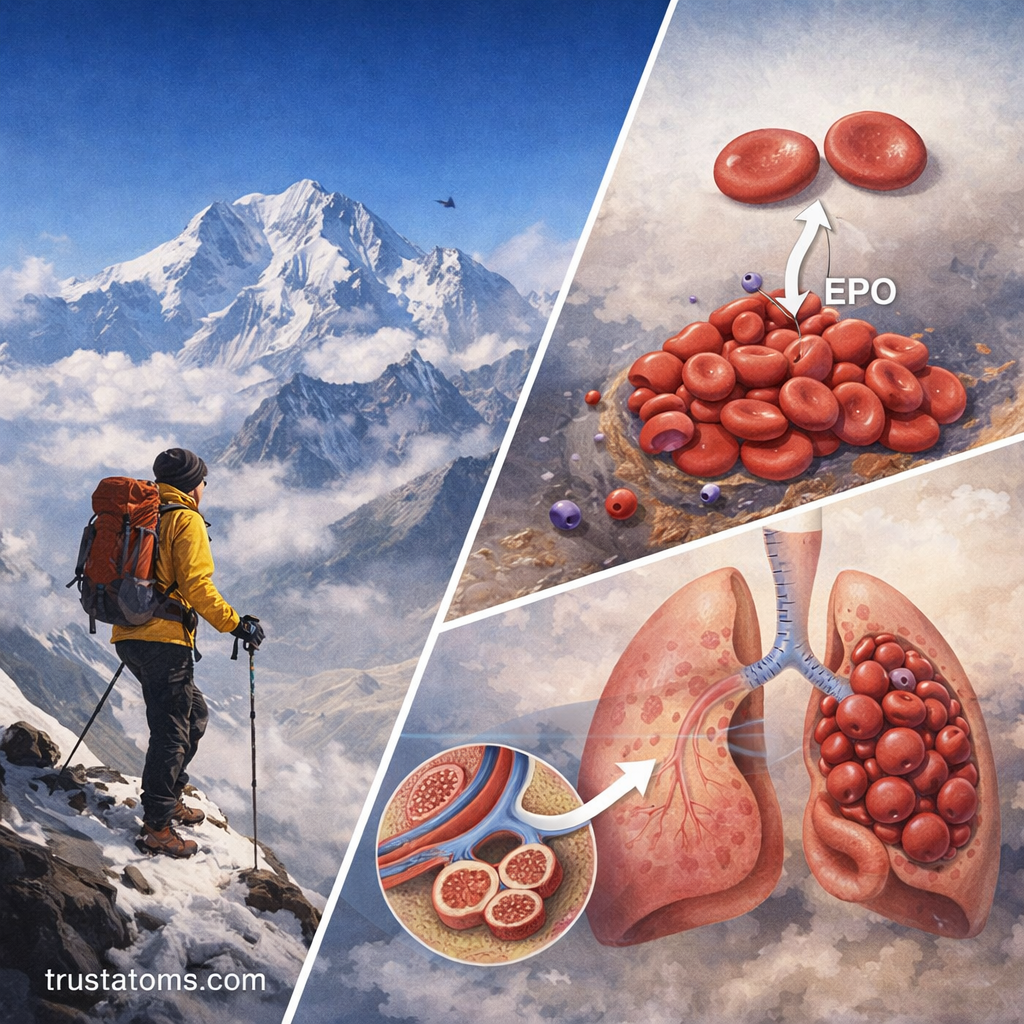
For individuals living at high altitude, the body undergoes more profound changes.
Increased Red Blood Cell Production
While technically part of the circulatory system, this adaptation directly supports respiration.
- The body produces more red blood cells
- Hemoglobin levels increase
- Oxygen-carrying capacity improves
This process is stimulated by the hormone erythropoietin (EPO).
Enhanced Oxygen Diffusion
The lungs become more efficient at transferring oxygen into the bloodstream:
- Capillary networks may expand
- Oxygen diffusion gradients improve
- Gas exchange becomes more effective
Structural Changes in the Respiratory System
In long-term high-altitude residents (such as those in the Andes or Himalayas), structural adaptations may occur.
These can include:
- Larger lung volumes
- Increased chest size
- Greater surface area for gas exchange
These changes are especially noticeable in populations that have lived at altitude for generations.
Cellular and Molecular Adaptations
Beyond organs and systems, the body also adapts at a microscopic level.
Increased Mitochondrial Efficiency
Cells may:
- Use oxygen more efficiently
- Produce energy with less oxygen
Upregulation of Hypoxia-Inducible Factors (HIF)
HIF proteins help regulate genes involved in:
- Red blood cell production
- Blood vessel formation
- Oxygen utilization
These molecular changes improve survival in low-oxygen environments.
Acclimatization vs. Adaptation
It’s important to distinguish between two key terms:
Acclimatization (Short-Term)
- Occurs over days to weeks
- Reversible
- Experienced by travelers or climbers
Adaptation (Long-Term)
- Occurs over generations
- Genetic in nature
- Seen in high-altitude populations
Common Challenges at High Altitude
Despite these adaptations, the body may still struggle.
Acute Mountain Sickness (AMS)
Symptoms include:
- Headache
- Nausea
- Fatigue
- Shortness of breath
High-Altitude Pulmonary Edema (HAPE)
A serious condition where fluid accumulates in the lungs, impairing gas exchange.
High-Altitude Cerebral Edema (HACE)
Swelling of the brain due to hypoxia—this is life-threatening and requires immediate descent.
Tips for Safe High-Altitude Exposure
If you’re planning to travel or train at high altitude:
- Ascend gradually (no more than 300–500 meters per day above 2,500 m)
- Stay hydrated
- Avoid alcohol early on
- Allow time for acclimatization
- Recognize early symptoms of altitude sickness
Why These Adaptations Matter
Understanding respiratory adaptations at high altitude has practical and scientific importance:
- Helps mountaineers and athletes perform safely
- Guides medical treatment for hypoxia-related conditions
- Provides insight into human evolution and resilience
- Supports aviation and space physiology research
Final Thoughts
The human body is remarkably adaptable. From rapid breathing adjustments to long-term structural and cellular changes, our respiratory system works tirelessly to maintain oxygen balance—even in the most challenging environments.
Whether you’re hiking in the mountains or studying human physiology, high-altitude adaptation is a powerful example of how the body responds to environmental stress.