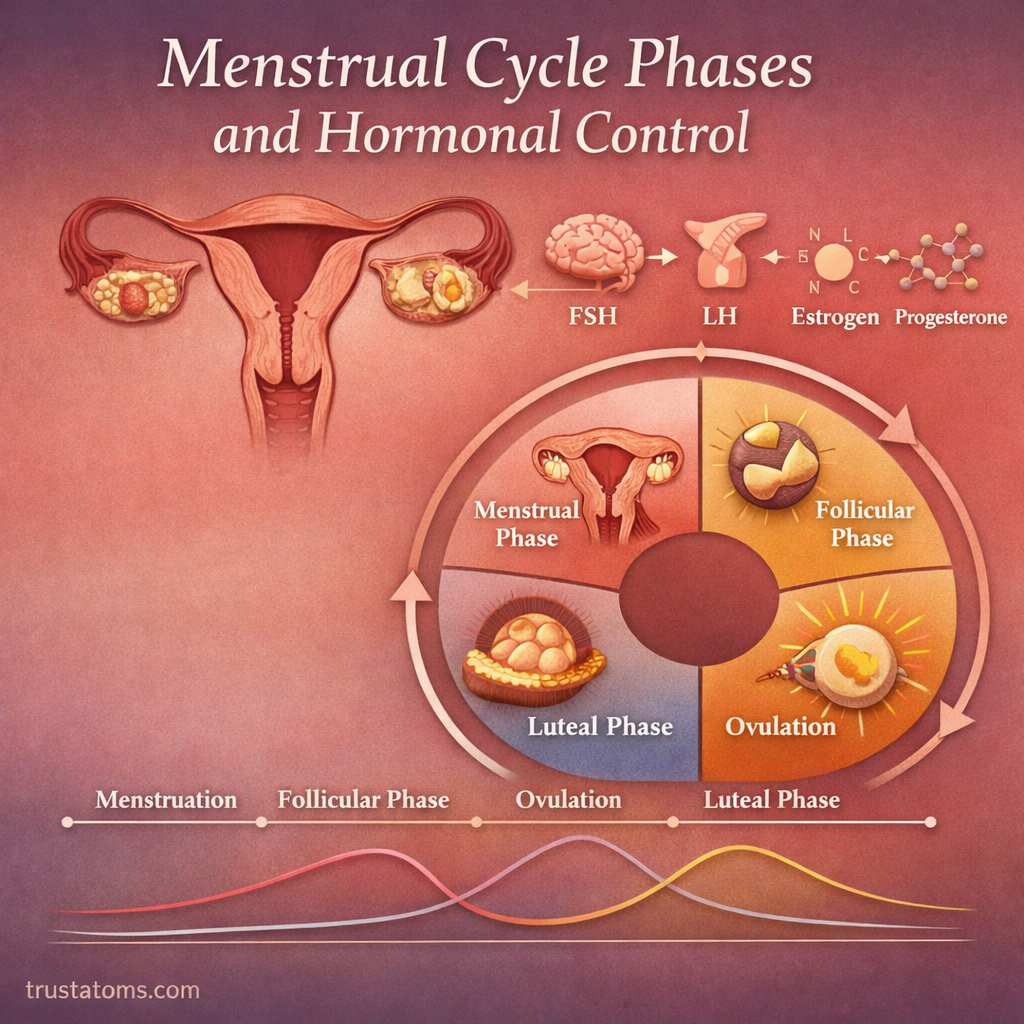
The menstrual cycle is a coordinated series of physiological changes in the female body that prepares it for potential pregnancy. Controlled by a complex interaction of hormones, the cycle typically lasts about 28 days (though 21–35 days is normal for adults).
Understanding the phases of the menstrual cycle and the hormones that regulate them is essential for learning about reproductive health, fertility, and overall hormonal balance.
Overview of the Menstrual Cycle
The menstrual cycle is divided into four main phases:
- Menstrual Phase
- Follicular Phase
- Ovulation
- Luteal Phase
Each phase is driven by hormonal signals between the brain and the ovaries, primarily involving:
- Estrogen
- Progesterone
- Follicle-stimulating hormone (FSH)
- Luteinizing hormone (LH)
These hormones are regulated through the hypothalamus-pituitary-ovarian (HPO) axis.
1. Menstrual Phase (Days 1–5)
The menstrual phase marks the beginning of the cycle and is defined by the shedding of the uterine lining (endometrium).
What Happens
- The uterus sheds its inner lining, resulting in menstrual bleeding
- Hormone levels (estrogen and progesterone) are low
- The body resets for a new cycle
Hormonal Activity
- Decreased estrogen and progesterone trigger menstruation
- The pituitary gland begins releasing FSH to stimulate follicle development
Key Point
This phase represents the body’s way of eliminating the previous cycle’s unused uterine lining.
2. Follicular Phase (Days 1–13)
The follicular phase overlaps with menstruation at the beginning but continues after bleeding stops.
What Happens
- The ovaries develop multiple follicles (each containing an immature egg)
- One follicle becomes dominant
- The uterine lining begins to rebuild
Hormonal Activity
- FSH stimulates follicle growth in the ovaries
- Growing follicles release estrogen
- Estrogen thickens the endometrium
Key Point
Rising estrogen levels prepare the uterus for potential implantation and signal the body to move toward ovulation.
3. Ovulation (Around Day 14)
Ovulation is the release of a mature egg from the ovary.
What Happens
- The dominant follicle releases an egg into the fallopian tube
- The egg is available for fertilization for about 12–24 hours
Hormonal Activity
- A surge in LH triggers ovulation
- Estrogen peaks just before ovulation
Key Point
Ovulation is the most fertile window of the cycle. If sperm is present, fertilization can occur.
4. Luteal Phase (Days 15–28)
The luteal phase begins after ovulation and ends when the next menstrual cycle starts.
What Happens
- The empty follicle transforms into the corpus luteum
- The uterus prepares for possible implantation
- If fertilization does not occur, the cycle resets
Hormonal Activity
- Progesterone is released by the corpus luteum
- Progesterone maintains the uterine lining
- If pregnancy does not occur, progesterone levels fall
Key Point
The drop in progesterone triggers the breakdown of the uterine lining, leading back to menstruation.
Hormonal Control of the Cycle
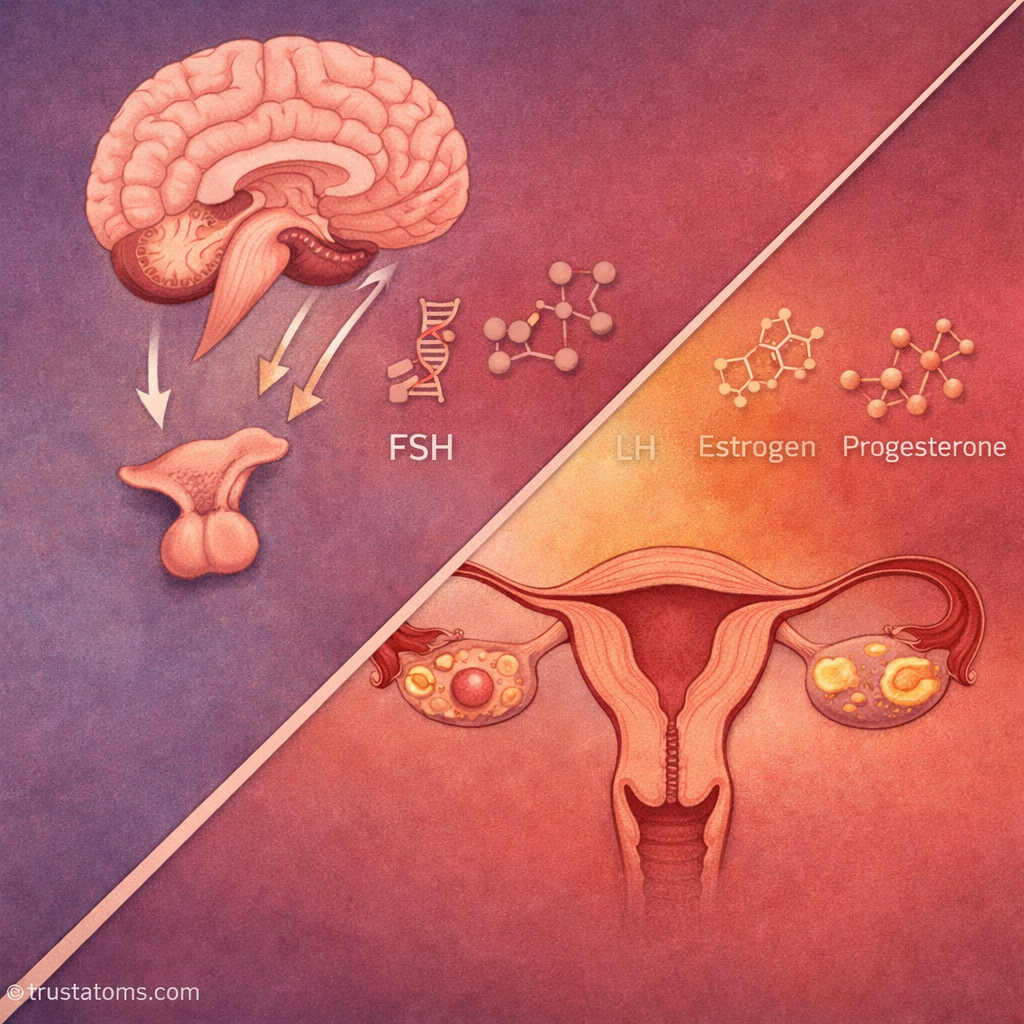
The menstrual cycle is regulated by a feedback system involving the brain and reproductive organs.
The Hormonal Pathway
- The hypothalamus releases gonadotropin-releasing hormone (GnRH)
- GnRH stimulates the pituitary gland
- The pituitary releases FSH and LH
- The ovaries produce estrogen and progesterone
- These hormones provide feedback to the brain
Hormonal Roles Summary
- Estrogen: Builds and thickens the uterine lining
- Progesterone: Maintains the lining for implantation
- FSH: Stimulates follicle development
- LH: Triggers ovulation
How Hormones Interact (Feedback Loops)
Hormonal control relies on feedback mechanisms:
Negative Feedback
- High estrogen and progesterone suppress FSH and LH
- Prevents multiple ovulations
Positive Feedback
- A sharp rise in estrogen triggers the LH surge
- Leads to ovulation
Key Insight
These feedback loops ensure that the cycle progresses in a controlled and timed manner.
Common Variations in the Menstrual Cycle
Not all cycles follow a strict 28-day pattern. Variations can occur due to:
- Age (e.g., adolescence or perimenopause)
- Stress levels
- Hormonal imbalances
- Lifestyle factors (diet, exercise)
Typical Ranges
- Cycle length: 21–35 days
- Menstrual duration: 3–7 days
Irregularities are common but may require evaluation if persistent.
Why Understanding the Cycle Matters
Learning about menstrual phases and hormonal control can help:
- Track fertility and ovulation
- Recognize normal vs. abnormal patterns
- Understand symptoms like cramps, mood changes, or fatigue
- Improve reproductive health awareness
Final Thoughts
The menstrual cycle is a finely tuned biological process regulated by hormonal signals between the brain and ovaries. Each phase plays a specific role in preparing the body for pregnancy, even if pregnancy does not occur.
By understanding these phases and the hormones involved, individuals can better interpret their bodies, monitor changes, and make informed decisions about their health.