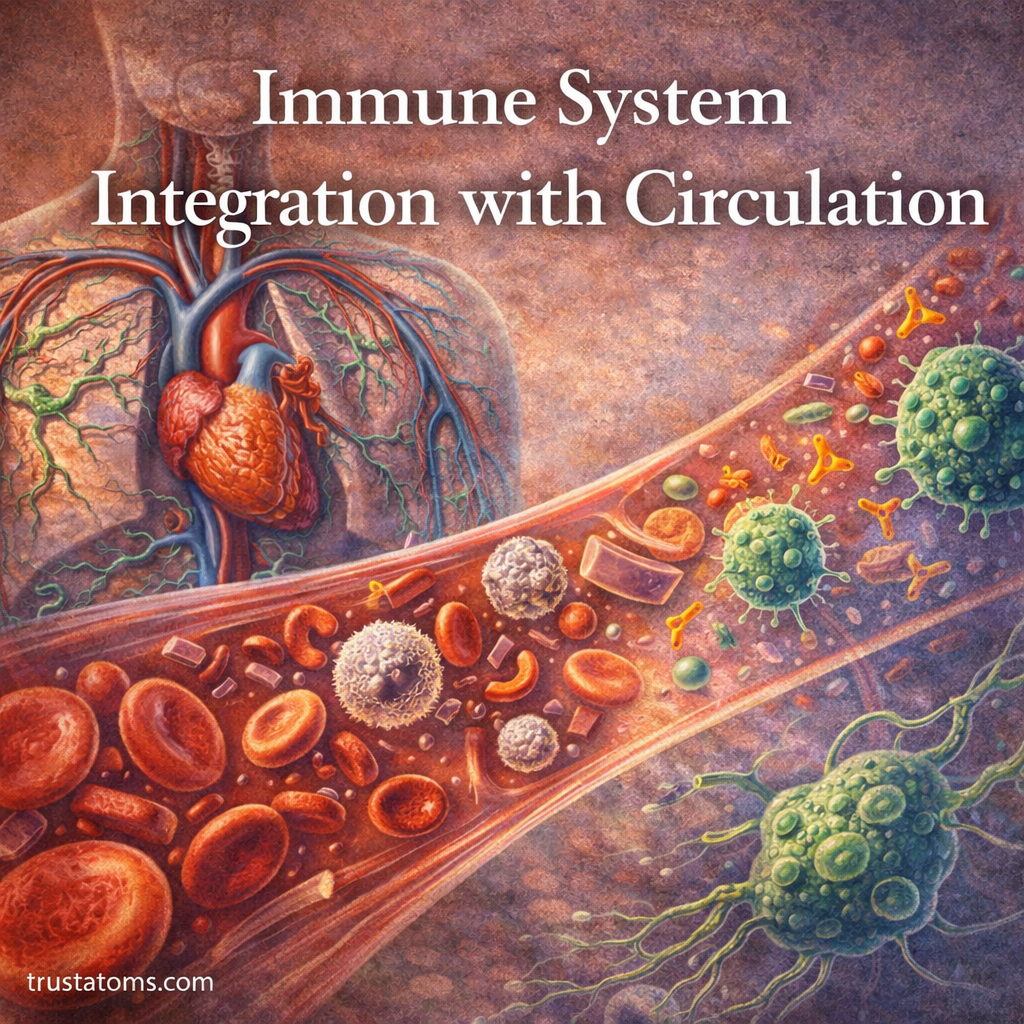
The immune system does not operate in isolation. It relies heavily on the circulatory system to move cells, signals, and molecules throughout the body. This integration allows the body to detect threats quickly, coordinate responses, and deliver immune defenses exactly where they are needed.
Understanding how the immune system works with circulation reveals how the body maintains constant surveillance against infection and injury.
Why Circulation Is Essential for Immunity
The circulatory system acts as a transportation network for immune components. Without it, immune cells would not be able to reach infection sites efficiently.
Key Functions of Circulation in Immunity
- Transports white blood cells to areas of infection
- Distributes signaling molecules like cytokines
- Carries antibodies throughout the body
- Removes waste products and pathogens
This constant movement ensures rapid detection and response to threats.
Components of the Circulatory System in Immune Function
Several parts of the circulatory system play direct roles in immune activity.
Blood
Blood is the primary medium for immune transport.
Key Immune Components in Blood
- White blood cells (leukocytes): Fight infections
- Plasma proteins: Include antibodies and complement proteins
- Cytokines: Coordinate immune signaling
Blood allows these elements to circulate continuously, providing full-body protection.
Lymphatic System
The lymphatic system works alongside the circulatory system to support immunity.
Key Roles of the Lymphatic System
- Drains excess fluid from tissues
- Transports immune cells
- Filters pathogens through lymph nodes
Lymph nodes act as checkpoints where immune responses can be activated.
Blood Vessels
Blood vessels are more than just passive pathways.
Their Role in Immunity
- Expand (vasodilation) to increase blood flow during infection
- Become more permeable to allow immune cells to exit into tissues
- Direct immune cells to specific sites of inflammation
This controlled movement is essential for targeted immune responses.
How Immune Cells Travel Through the Body
Immune cells are constantly moving, even when no infection is present.
The Surveillance Process
- Immune cells circulate in the bloodstream
- They monitor for signs of infection or damage
- When activated, they adhere to blood vessel walls
- They exit the bloodstream into affected tissues
This process is known as immune surveillance, ensuring rapid detection of threats.
The Role of Inflammation in Circulatory Integration
Inflammation is a key mechanism that connects immune activity with circulation.
What Happens During Inflammation
- Blood vessels dilate, increasing blood flow
- Vessel walls become more permeable
- Immune cells migrate into tissues
Visible Effects
- Redness (increased blood flow)
- Heat (elevated circulation)
- Swelling (fluid and cell accumulation)
- Pain (pressure on surrounding tissues)
Inflammation ensures that immune resources are concentrated where they are needed most.
Cytokines and Chemical Signaling
Cytokines are chemical messengers that travel through the bloodstream to coordinate immune responses.
Functions of Cytokines
- Signal immune cells to activate or move
- Regulate inflammation
- Coordinate systemic responses like fever
These signals allow the immune system to communicate across the entire body.
Antibodies and Circulatory Distribution
Antibodies are produced by B cells and released into the bloodstream.
How Circulation Enhances Antibody Function
- Distributes antibodies to all tissues
- Allows rapid binding to pathogens
- Helps neutralize toxins and bacteria
Because of circulation, antibodies can act far from where they were produced.
Interaction Between Blood and Lymph
The blood and lymphatic systems are closely connected.
How They Work Together
- Fluid from blood enters tissues as interstitial fluid
- This fluid becomes lymph and carries immune cells
- Lymph is filtered in lymph nodes
- Cleaned fluid returns to the bloodstream
This cycle ensures continuous monitoring and filtration of potential threats.
The Role of Organs in Immune Circulation
Certain organs play specialized roles in integrating immunity with circulation.
Key Organs
- Spleen: Filters blood and removes pathogens
- Bone marrow: Produces immune cells
- Lymph nodes: Activate immune responses
These organs act as hubs where immune cells are produced, activated, or filtered.
When Integration Becomes Dysregulated
While this system is highly effective, problems can occur when coordination breaks down.
Potential Issues
- Poor circulation can delay immune responses
- Excess inflammation can damage tissues
- Overactive immune signaling can lead to autoimmune conditions
Maintaining balance is essential for proper immune function.
Final Thoughts
The integration of the immune system with circulation is essential for survival. Through the constant movement of cells, signals, and proteins, the body maintains a state of readiness against infection and injury.
From immune surveillance to targeted inflammation, this partnership ensures that defenses are both rapid and precise. Understanding this connection highlights the importance of circulation not just for oxygen delivery—but for immune protection as well.