Bacteria are everywhere—on surfaces, in the air, and even inside the human body. While many are harmless or beneficial, harmful bacteria can cause infections if they enter the body. To prevent this, the immune system relies on a multi-layered set of antibacterial defense mechanisms designed to block, detect, and eliminate bacterial threats.
These defenses work together across physical barriers, rapid immune responses, and highly targeted adaptive immunity.
What Makes Bacteria Different from Other Pathogens?
Bacteria are living, single-celled organisms capable of reproducing independently. Unlike viruses, they do not need to invade cells to multiply.
Key Characteristics of Bacteria
- Can live and reproduce outside host cells
- Often produce toxins that damage tissues
- Can form colonies and biofilms
- Typically larger than viruses, making them easier to detect
Because bacteria often exist outside cells, the immune system can directly attack them in the bloodstream and tissues.
The Three Lines of Antibacterial Defense
The body protects itself through three major layers of defense:
1. Physical and Chemical Barriers
Prevent bacteria from entering the body.
2. Innate Immune Response
Provides rapid, non-specific defense.
3. Adaptive Immune Response
Delivers targeted and long-lasting protection.
Physical and Chemical Barriers
The first line of defense stops bacteria before they can cause harm.
Skin: The Protective Shield
- Acts as a physical barrier to bacterial entry
- Produces antimicrobial substances
- Maintains a slightly acidic environment that inhibits bacterial growth
Mucous Membranes and Secretions
These line the respiratory, digestive, and urinary tracts.
Key Protective Mechanisms
- Mucus traps bacteria
- Cilia move trapped particles out of the body
- Tears and saliva contain antibacterial enzymes like lysozyme
Stomach Acid and Microbiota
- Stomach acid destroys many ingested bacteria
- Beneficial bacteria (microbiota) compete with harmful species
This prevents harmful bacteria from establishing infections.
Innate Antibacterial Defense Mechanisms
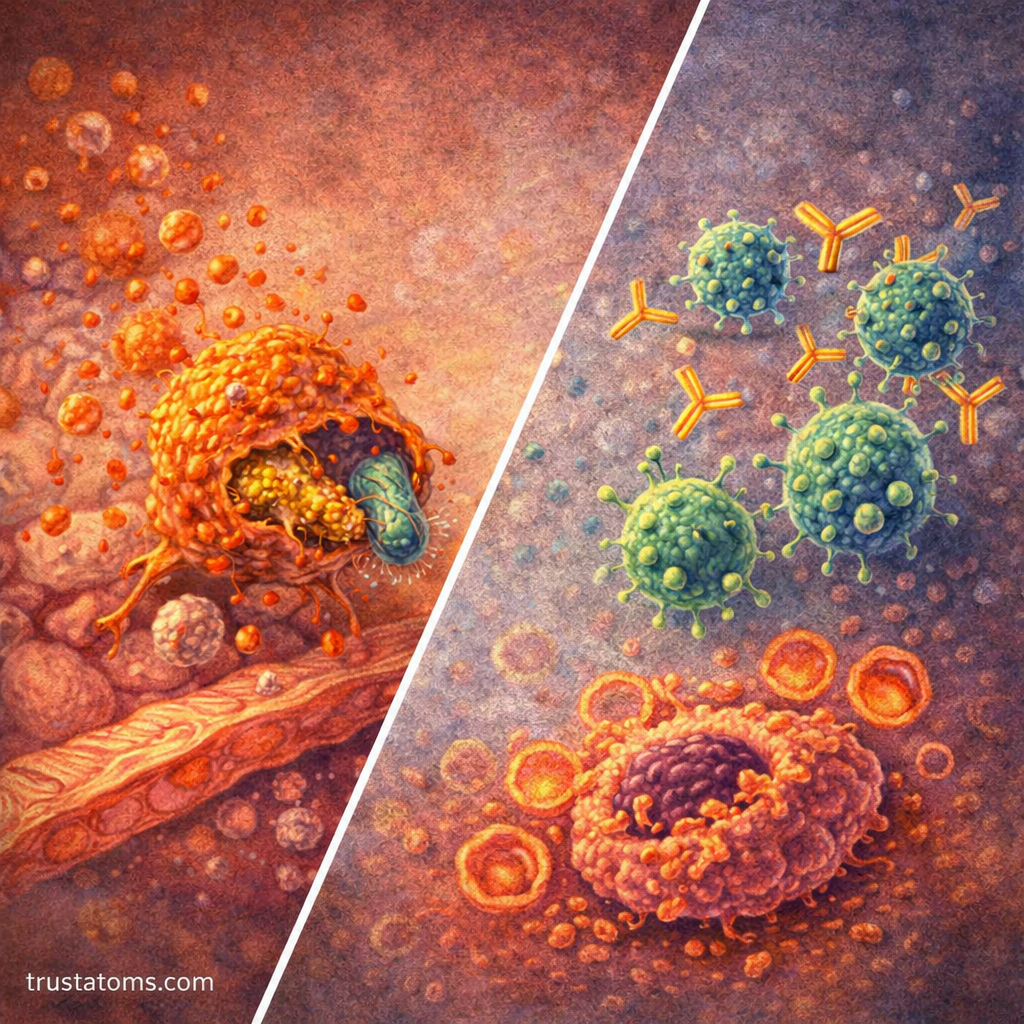
If bacteria breach initial barriers, the innate immune system responds immediately.
Phagocytes: The Bacteria Engulfers
Phagocytes are immune cells that ingest and destroy bacteria.
Types of Phagocytes
- Neutrophils: First responders that rapidly attack bacteria
- Macrophages: Long-lived cells that clean up pathogens and debris
How Phagocytosis Works
- Detection of bacteria
- Engulfment into a vesicle
- Digestion using enzymes
- Removal of waste
This process is one of the most effective ways to eliminate bacteria.
Inflammation: The Local Response
Inflammation is a key feature of antibacterial defense.
Signs of Inflammation
- Redness
- Swelling
- Heat
- Pain
What Inflammation Does
- Increases blood flow to infected areas
- Brings immune cells to the site
- Enhances the destruction of bacteria
Complement System
The complement system is a group of proteins in the blood that help eliminate bacteria.
Functions of the Complement System
- Marks bacteria for destruction (opsonization)
- Forms membrane attack complexes that rupture bacterial cells
- Enhances inflammation
This system amplifies the immune response and improves efficiency.
Adaptive Antibacterial Defense Mechanisms
If bacteria persist, the adaptive immune system provides a targeted response.
B Cells and Antibody Production
B cells produce antibodies that bind specifically to bacterial antigens.
Functions of Antibodies
- Neutralize bacterial toxins
- Mark bacteria for phagocytosis
- Activate the complement system
Antibodies make it easier for the immune system to identify and eliminate bacteria.
T Cells: Coordinating the Response
While T cells are more commonly associated with viral defense, they also play roles in bacterial infections.
Key Roles of T Cells
- Helper T cells (CD4+) activate B cells and macrophages
- Support inflammation and immune coordination
- Help control intracellular bacteria
The Role of Fever in Antibacterial Defense
Fever is a common response to bacterial infection.
How Fever Helps
- Slows bacterial growth
- Enhances immune cell activity
- Promotes production of immune proteins
This systemic response supports the body’s ability to fight infection.
Bacterial Evasion Strategies
Some bacteria have evolved ways to avoid immune detection.
Common Strategies
- Forming protective capsules
- Producing enzymes that break down immune signals
- Hiding within host cells
- Developing resistance to antibiotics
These adaptations can make infections more difficult to treat.
Balancing the Immune Response
An effective antibacterial response must be carefully regulated.
If the Response Is Too Weak
- Infection spreads
- Bacterial growth increases
If the Response Is Too Strong
- Excess inflammation damages tissues
- Can lead to conditions like sepsis
The immune system must strike a balance between eliminating bacteria and protecting the body.
Final Thoughts
Antibacterial defense mechanisms are a complex and highly coordinated system involving physical barriers, rapid immune responses, and targeted adaptive immunity. From the skin’s protective barrier to phagocytes engulfing bacteria and antibodies marking them for destruction, the body uses multiple strategies to stay protected.
Understanding these defenses highlights how the immune system constantly works to maintain health and prevent infection in a world full of microbial threats.